Clinician Burnout Crisis in the Era of COVID-19: Insights from the Frontlines of Care
 The NAM continues to stand with health workers, throughout the COVID-19 pandemic and beyond.
The NAM continues to stand with health workers, throughout the COVID-19 pandemic and beyond.
Read a National Plan for Health Workforce Well-Being >>
Hear more about uniting the health workforce to optimize well-being, and developing actionable strategies to retain clinicians >>
Burnout is a workplace syndrome characterized by high emotional exhaustion, high depersonalization, and a low sense of personal accomplishment from work. COVID-19 has presented clinicians with even greater workplace hardships and stressed an already broken system that resulted in an unsustainable working environment for clinicians.
In April 2021, the National Academy of Medicine’s (NAM) Action Collaborative on Clinician Well-Being and Resilience (Clinician Well-Being Collaborative) reached out to their network and received over 500 questionnaire responses on the effects of the pandemic on clinicians’ personal and professional lives. Respondents also shared creative solutions implemented by health care organizations to better support their workforce approximately one year into the pandemic.
Respondents saw systems change as a fundamental step to creating an environment in which clinicians can feel good about going to work and joining the health workforce.
If you or a loved one is feeling distressed, the National Suicide Prevention Lifeline provides free and confidential emotional support 24 hours a day, 7 days a week.
Call or text the National Suicide Prevention Lifeline at 988.
The NAM offers these topline takeaways as a snapshot of frontline clinicians’ lived experiences, and a resource to help inform our movement to enhance clinician well-being.
1. Clinicians experienced trauma and burnout specific to COVID-19 on top of existing large scale system pressures and alarming stress levels among the health care workforce.
In addition to witnessing firsthand the numerous deaths caused by the pandemic, unique factors that contributed to clinician burnout during COVID-19 included: the burden of keeping up with constantly changing safety guidelines, equipment shortages, and a lack of certainty regarding treatment options. Explicit allusions to war by respondents illustrated the personal cost to clinicians from the loss of their colleagues and patients, and highlighted the moral injury and detrimental effects on well-being felt by caregivers unable to fulfill their values.




2. The manifestation of burnout varied across clinicians—ranging from depression to anxiety to moral distress.
Some respondents described their burnout in matter-of-fact terms, seeing it as a natural result of a once-in-a-generation pandemic and a stimulus for self-reflection and growth. Other respondents expressed feelings of helplessness when describing their burnout. Overall, there was an understanding that clinicians needed to take care of themselves—despite some not knowing how to start or a recognition that traditional avenues of easing burnout like exercising, socializing, or spending time with loved ones were virtually impossible because of a lack of time and/or social distancing measures.




3. Health care workers were not immune to the impacts of COVID-19 in their professional or personal lives, and expressed frustrations with the dearth of chances to connect with their peers and thrive in their roles.
Respondents noted that they put research projects, teaching opportunities, and manuscripts on hold due to the all-encompassing nature of COVID-19 response. Other respondents shared that the task of caring for COVID-19 patients limited the already scarce time they had with friends and family, and any downtime they had was dominated by a sense of exhaustion, putting strain on relationships. Respondents highlighted impacts on parenting and challenges of juggling other work-life responsibilities.




4. Efforts made by hospitals and other health care organizations to address burnout were generally viewed positively, but clinicians who didn’t feel supported expressed their desire for more interventions by their organizations.
Respondents mentioned group therapy, town halls, confidential one-on-one counseling sessions, peer support, post-shift debrief sessions, the ability to telework, and time off from seeing patients as helpful ways in which their employers sought to address burnout. Proactive outreach by their employers—rather than spending their limited personal time off to navigate mental health and support services—was noted as a big help. Others identified a lack of open communication—particularly from their organizational leadership—as well as a need for more transparency around help-seeking. Clinicians responding to the questionnaire expressed hope that an environment of openness and support continues to grow after the pandemic, both within those institutions progressing in the right direction and across all organizations.




5. Clinicians expressed the need for burnout interventions implemented during COVID-19 to continue post-pandemic.
Most respondents wanted their leadership to support widespread cultural change in which systems prioritize clinician well-being (both mental and physical health, and where solutions are implemented upstream at a system level rather than ad hoc, individual interventions). While noting that these solutions aren’t cure-alls, respondents wanted many of the employer interventions that demonstrated success during the pandemic to become permanent efforts to mitigate burnout.




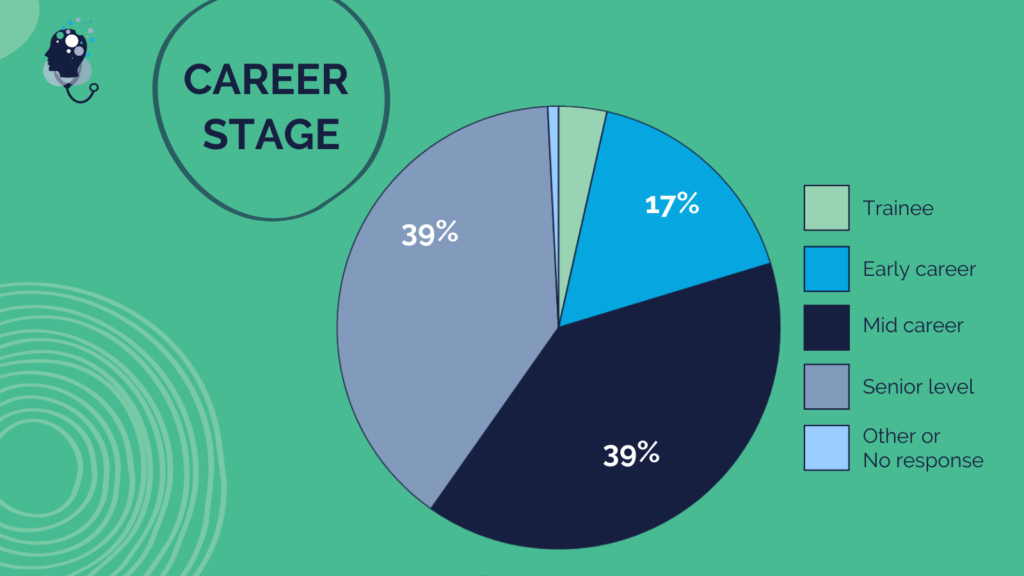
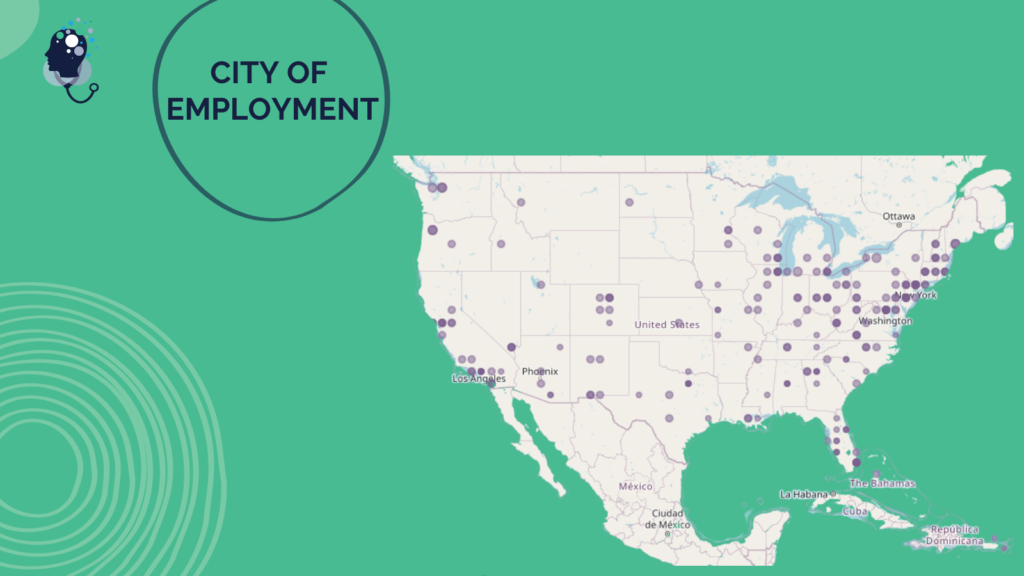
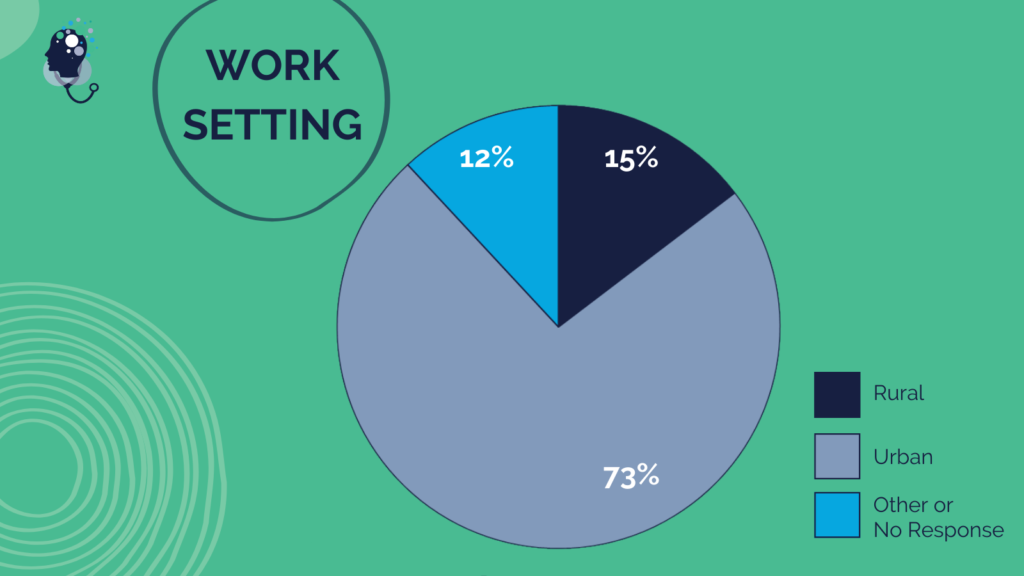
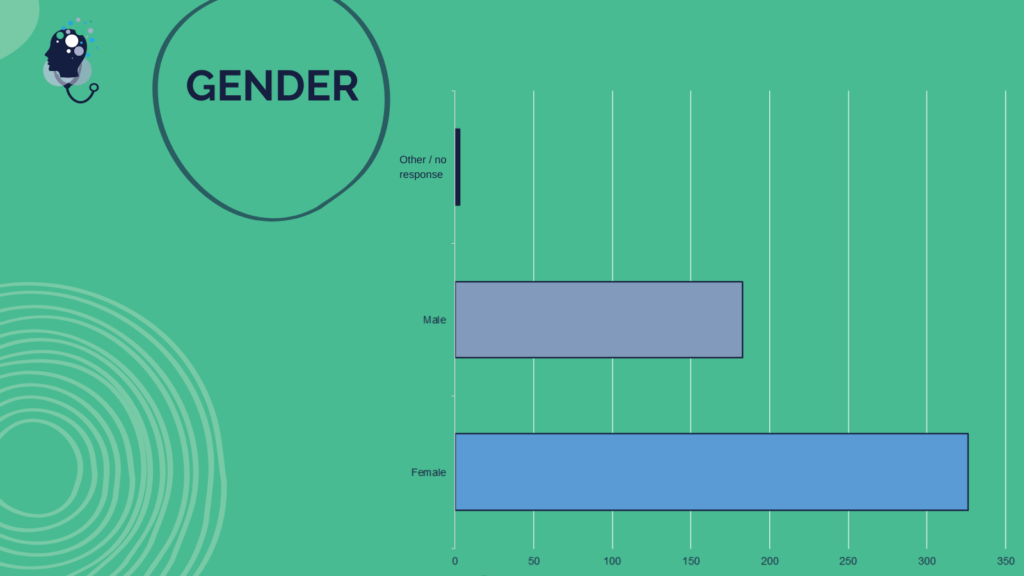
Questionnaire Respondent Demographics Overview
Questionnaire respondents hailed from health care communities across the U.S., providing a broad range of perspectives and experiences from different health professions and career stages, and a diversity of races, ethnicities, and genders. The following graphics describe the self-reported demographics of all respondents.


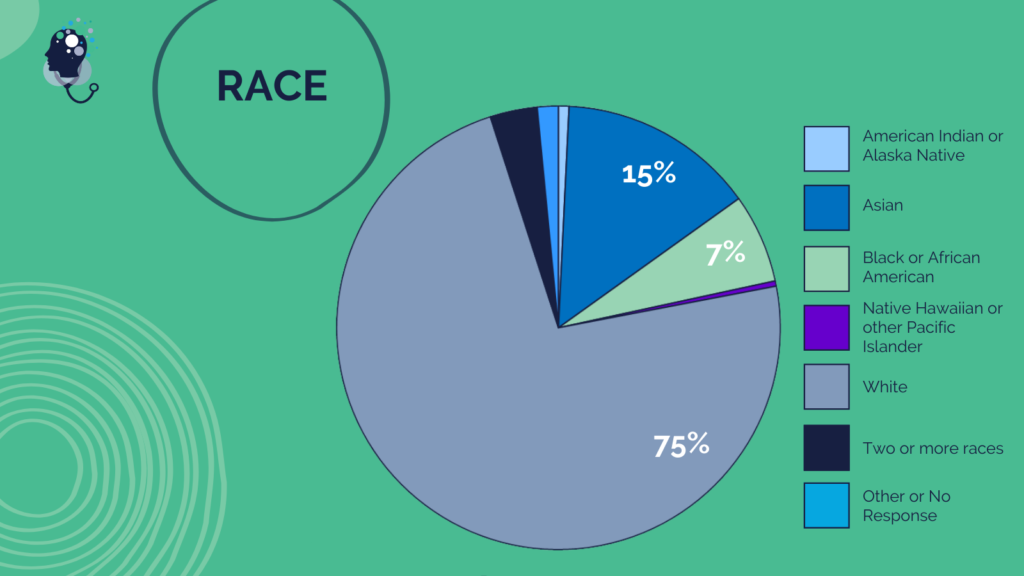
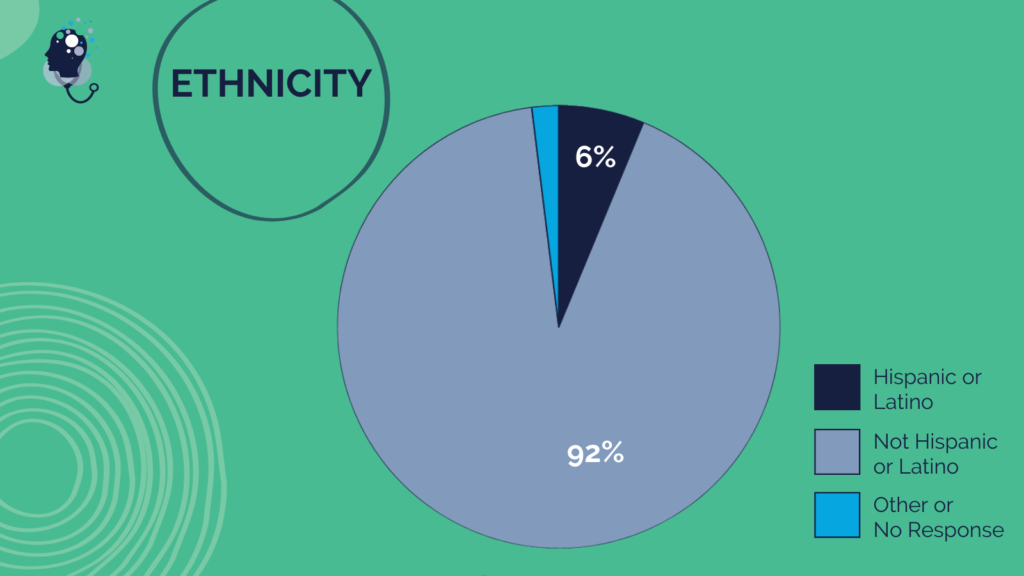
Note: This was prepared as a summary of individual questionnaire responses and key themes. The statements made are those of individual respondents and do not necessarily represent the views of all respondents; members of the Action Collaborative on Clinician Well-Being and Resilience; the National Academy of Medicine; or the National Academies of Sciences, Engineering, and Medicine.
This product is part of ongoing efforts to hear and amplify clinician stories, and have their experiences and insights inform activities of the Clinician Well-Being Collaborative. The questionnaire responses were used to inform an invitation-only NAM listening session in April 2021 that U.S. Surgeon General Vivek Murthy joined, during which frontline clinicians offered their personal stories about the impacts of burnout.
Related Products


