Kelly J. Clark
Alex Woodruff
Jean Glossa
Andrey Ostrovsky
the Prevention
Treatment
Recovery Working Group of the Action Collaborative on Countering the U.S. Opioid Epidemic


Introduction
The United States is in the midst of a multifactorial drug overdose and death epidemic. In 2020, over 80,000 deaths [15] in the U.S. were attributed to drug overdose, more than 50,000 of which were opioid-related. This is an increase of roughly 10 percent from 2018, when nearly twice the number of people died from a drug overdose than died from HIV/AIDS at the peak of that epidemic in 1995 [51]. According to recent estimates, with nicotine included, over 35 million people have a substance use disorder (SUD) (14 percent of the U.S. population), and roughly 10.1 million people reported opioid misuse or any heroin use in the previous year [14].
The epidemic of drug, and especially opioid-related, overdose deaths has been declared a national public health emergency since 2017. What is needed to turn the tide of this epidemic is a long-term, sustainable approach to preventing and managing addiction as a chronic disease that will replace America’s current approach of lurching from one crisis to the next. Coordinated, compassionate, and science-based care is necessary. Despite research on the individual, societal, carceral, and economic factors that created the epidemic, public policy and treatment resources have been unable to keep up with its trajectory [26]. The effects of drug use, ill-informed drug policies, addiction, and overdose continue to devastate people across the United States—particularly Black, Latinx, Native American, LGBTQ+, and other traditionally marginalized communities. Models observing the course of the drug overdose epidemic predict that without treatment expansion, another 400,000 people will die from overdose by 2025 [17]. The COVID-19 pandemic has further exacerbated the opioid epidemic [52]. Many counties across the U.S. have reported disruptions in public health programs essential to people who use drugs, disruptions to transportation to treatment providers, and ongoing challenges in accessing evidence-based care because of inadequate access to quality treatment providers [52]. Moreover, the SUD treatment system should be adapted to better engage and educate patient family members and support networks about their loved ones’ treatment plans. There is a clear need for future-oriented strategies to build a robust addiction treatment system that ensures widespread access to treatment.
Overcoming the drug overdose epidemic will require identifying and addressing critical gaps across the SUD treatment system. The majority of U.S. states, counties, and municipalities do not strategically distribute funding across the SUD treatment landscape. To appropriately align funding to needs across the treatment system and invest in training adequate numbers of new providers of multiple disciplines, the following are needed: a technical assessment of the local SUD treatment system and administrative time to contract with state vendors; development of data-release processes; and organization of the reporting structures associated with state, county, and municipality regulations. These burdens delay funding to organizations that would otherwise be poised to develop and execute programs for people with SUDs.
Individuals who encounter the justice system have significantly higher rates of opioid use than the general population and are at significantly higher risk of overdose upon leaving jail or prison than their peers who have not encountered the justice system [53]. This connection is obvious—people who experience SUDs may perform illegal activities to acquire their desired substance, and many of these substances are currently illegal [53]. This reality spotlights the failed history of America’s “war on drugs” and how the American criminal justice system currently operates. Any attempt to improve addiction care in the U.S. must include an expansion of assessment, treatment, and support for justice-involved populations based upon scientific data about best practices while considering the historic and systemic racism that has led to mass incarceration of Black individuals, particularly Black men [39,53].
Policymakers and health leaders have an opportunity to make targeted investments dedicated to repairing the damage done by the drug overdose epidemic and preventing further harm. To create a more robust and equitable medical system that recognizes and treats addiction, evidence-based interventions and programs need to be adequately funded and resourced. There also needs to be an effort to construct and enact the missing pieces of the currently fragmented system for treating addiction in the U.S. These investments and this new system all need to be developed and deployed while considering the pervasive impact of structural racism on how those with addiction are both viewed and treated (socially and medically). As such, it is incumbent upon those building this new system to evaluate and repair any laws, regulations, or payment structures that perpetuate this reality.
To ensure that funding is directed to aspects of the system that would most benefit from additional support, the authors of this paper propose the following architecture and guidance. The authors of this manuscript hope that this proposed guidance will help direct funding and action toward a robust, well-functioning SUD treatment system, but also recognize that much of the proposed guidance is most applicable to the treatment of opioid use disorder (OUD)—the major driver of overdose-related deaths.
The 4 Cs: Capacity, Competency, Consistency, and Compensation
To best describe the needs of and solutions for the addiction treatment ecosystem, the authors of this manuscript propose the guidance of the “4 Cs”: Capacity, Competency, Consistency, and Compensation.
Capacity refers to whether the system is correctly sized and nuanced enough to fill the needs of the community it is serving. The American Society of Addiction Medicine (ASAM) levels of care (LOCs) provide a useful framework to understand types of treatment called upon to treat SUD in a community [5]. Competency refers to the education, training, and evaluation of those who work within the treatment system, including but not limited to physicians, psychotherapists, administrators, and peer recovery specialists. Consistency refers to whether the system is delivering high-quality care. The quality of a system’s care is often assessed based on fidelity to best treatment practices and appropriate use of the system’s infrastructure. Compensation refers to whether the treatment system financially aligns reimbursement with best practices. Payment can be viewed through the lens of the payment amount, payment type, including whether payment is being made for evidence-based practice versus legacy treatment practices, and inclusion of carved-out versus carved-in behavioral health. While one could rightfully argue that a fifth “C” could be added for Community, that consideration is outside of the scope of this publication. The sections below explore each of these 4 Cs in detail.
Capacity
The disease of addiction, in all its forms, can affect and is affected by issues such as:
- early life trauma
- behavioral health needs
- biomedical needs
- psychiatric needs
- chronic pain
- withdrawal management needs
- housing
- food security
- transportation
- communication access
- cognitive capability
- cultural context
- criminogenic history and behavior
- structural racism
- a myriad of details for each named issue.
This manuscript acknowledges the complexity of the disease of addiction and attempts to discuss this disease in totality, but all of the interventions proposed in this paper will need to be rolled out with the whole patient, and all considerations outlined above, in mind.
The current state of the addiction treatment ecosystem is unable to manage and appropriately treat the millions of people with substance misuse, SUD, and addiction in the U.S. today. Because of the systemic barriers that make access to this care difficult, only a minority of patients receive evidence-based care [26], including medications for opioid use disorder (MOUD) and interventions for the social determinants of health-related issues listed above. Sufficient consideration of patients with chronic pain who develop a physical dependence to opioids or suffer from a SUD is also lacking. In addition to behavioral health treatment, these patients will require adequate management of their pain to facilitate improvement to their function and quality of life [69].
In many counties across the U.S., there are no addiction treatment facilities [22] even for those most severely afflicted with SUD—let alone those with mild to moderate SUD. In some counties, there may be an adequate number of addiction specialists, but health plans do not provide equitable or accessible care, despite the existence of the Mental Health Parity and Addiction Equity Act (MHPAEA) [16]. This Act and other parity-related legislation, such as the Affordable Care Act, have yet to be fully implemented and enforced. Developing effective monitoring and enforcement of mental health and SUD laws is a national imperative.
Despite multiple clear guidelines, the vast majority of Americans with addiction do not receive treatment inclusive of best practices, including MOUD. Many programs rely on abstinence-based treatment, which requires patients to forgo evidence-based medications that save lives [32]. This is particularly unfortunate given the medical and policy understanding that using these medications is consistent with both abstinence and recovery [54]. Given the need to focus on cost-effective and rapid solutions, it is imperative that funding is allocated to the types and LOCs that are aligned with the needs of patients in individual communities. For instance, the services unhoused patients need are different from those of people with stable housing, and the system should be responsive to those differing needs. This section will discuss capacity as it relates to the ASAM Continuum of Care, MOUD, workforce, telehealth, naloxone, and harm reduction services.
Capacity: ASAM Continuum of Care and the Treatment Ecosystem
The single most important concept in the treatment of patients with an OUD is the rapid and immediate initiation of MOUD followed by patient-centered and stigma-free services at the appropriate LOC. This means that while the medication is critical to rapidly stabilize a patient, it must be matched with the correct intensity of interventions that address all components of care listed above, including the relevant social determinants of health, to truly stabilize a patient in their recovery. For instance, consideration of patients’ access to secure housing and reliable transportation as well as their ability to afford care is critical in assessing the practical capacity of the treatment system. Without consistent access to care, availability of even the best treatment options will be inadequate.
The ASAM Criteria, formerly known as the ASAM Patient Placement Criteria, “is the most widely used and comprehensive set of guidelines for [service setting], continued stay, transfer, [and] discharge of patients with addiction and co-occurring conditions” [5]. When used correctly, the criteria guide the treatment provider through a six-dimensional biopsychosocial assessment (see Figure 1) that informs a comprehensive treatment plan. Once the needs of the patient are identified, an appropriate LOC can be chosen [4]. By identifying the areas where a patient’s support system is lacking or underdeveloped, addiction specialists can tailor interventions and service settings that would give the patient the best chance for stabilization.
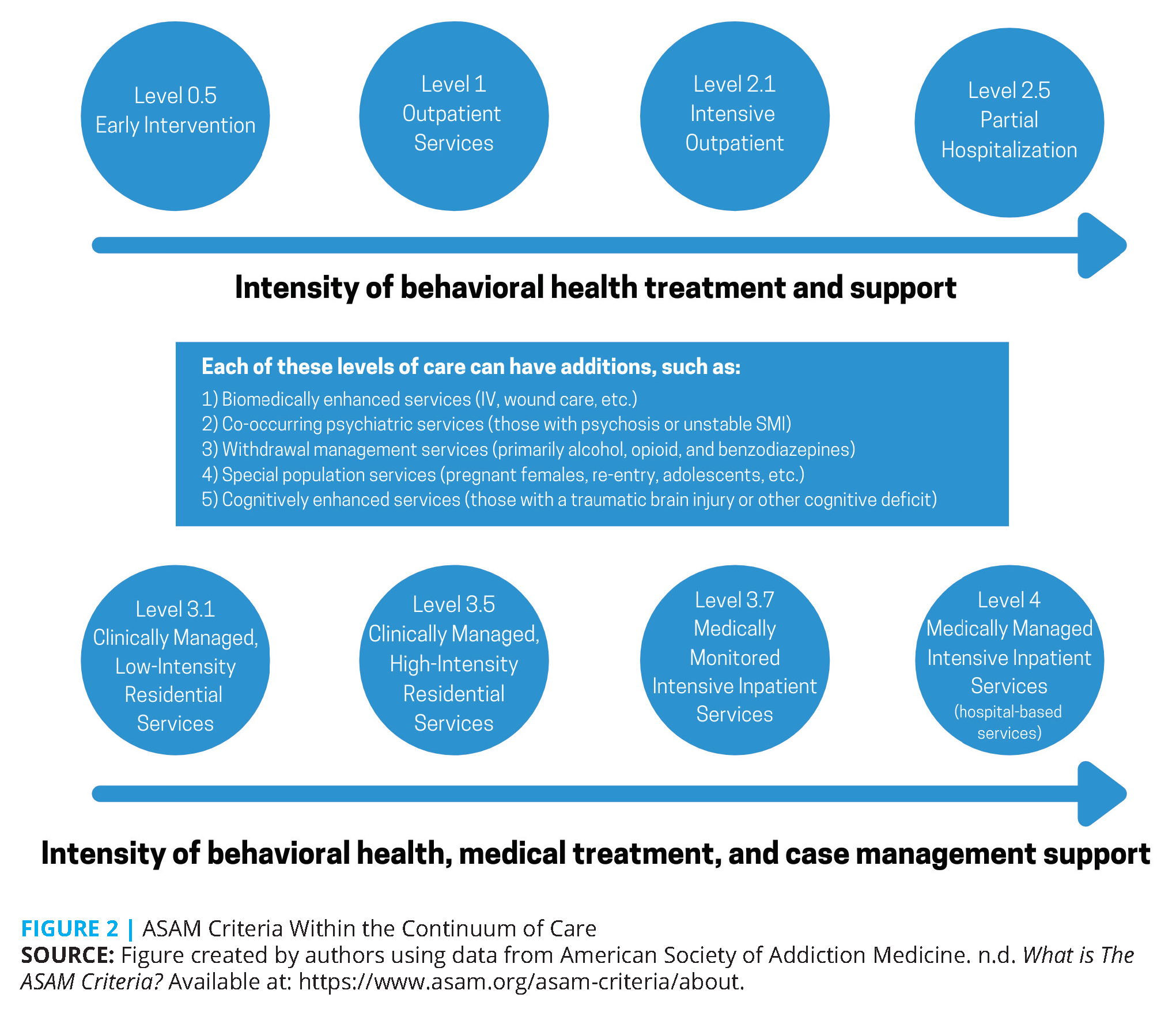
After the multidimensional assessment, patients are then recommended an ASAM Criteria LOC based on the assessment outcome and the needs identified in the treatment plan. Below, the authors of this manuscript briefly describe how each LOC, defined by the ASAM Criteria, fits into the continuum of treatment (see Figure 2).
Basic concepts should be employed while following the ASAM LOCs:
- U.S. Food and Drug Administration (FDA)-approved maintenance medications for addiction treatment should be made available at every LOC.
- Access to all needs associated with addiction treatment should be available either at the location (if specified by LOC) or by referral.
- These services (if not specified by otherwise) can be delivered telemetrically, via group practice or hub, and spoke methodology, via mobile units or even electronic applications.
- Currently the ASAM Criteria is in the process of its fourth revision. The descriptions below are forward-looking to this edition.
Level 0.5
Level 0.5 is the most basic of interventions and consists of modalities such as screening, brief assessment, brief intervention, and referral to treatment (SBIRT) or societal interventions, such as an impaired driving program for people who do not meet the diagnostic criteria for a SUD or addiction, but have high-risk driving behavior secondary to intoxication. This series of care tasks can, and should, occur in all areas of general medical care, including hospitals.
Level 1
Level 1 is designed to deliver services in a variety of locations and to a diverse subset of individuals. This LOC can be delivered at school-based clinics, mental health clinics, or primary care offices, and can be used for patients who are experiencing mild or moderate levels of addiction and are ready for a change or need ongoing addiction treatment. This could be an initial LOC or a step-down LOC for someone who is invested in recovery but is leaving residential treatment, or step-down treatment for someone who had intensive outpatient treatment. It can, and should, include referral for medications for addiction such as buprenorphine, naltrexone, or acamprosate, among many other choices. While the prescribing of medication for addiction treatment is of utmost importance, it is only part of the treatment and should not be delivered without some ability to address all needs in some fashion. There are fewer than nine hours of structured clinical services delivered by peers or addiction counselors provided at this LOC.
Example: A patient who meets criteria for level 1 services for OUD could have their medication written by a primary care physician who, if needed, refers the patient to a SUD counseling location.
Comprehensive Level 1
This LOC encompasses opioid treatment programs (OTPs/methadone clinics) and comprehensive office-based opioid treatment providers (OBOT). OTPs are heavily regulated and provide both medication and behavioral health services on site or in close coordination. They can provide varying levels of intensity for clinical services on-site and have some grouping of counselors and licensed staff available for both individual and group therapies. OTPs can and generally do use all forms of MOUD. OBOTs are outpatient offices that use only buprenorphine and naltrexone for OUD. However, buprenorphine is a controlled substance, highly regulated by the Drug Enforcement Administration (DEA). At the time of this publication, prescribers must have a DEA waiver to prescribe buprenorphine and meet the state’s requirements for prescribing this medication [20]. They need to either deliver on-site
behavioral therapy or have the ability to refer out to behavioral therapy. There should also be access to primary care services, either in-house or by referral, at this LOC.
Example: A patient who is being treated at a comprehensive level 1 will need more substantial medication monitoring (daily dosing or short-term prescriptions) and closer coordination with case management and behavior services. The addition of peer support and more comprehensive toxicological evaluations should be the norm.
Level 2.1 and 2.5
Level 2.1 Intensive Outpatient
This LOC must support medical, psychiatric, psychological, laboratory, and toxicology services through direct care, through telemedicine, or by referral. They should have emergency services available 24 hours per day and have direct access to the other LOCs. This LOC provides nine hours or more of programed clinical intervention per week. A patient would continue services here until they are ready to step down to a less intensive LOC or are moved to a more intensive LOC because of increasing severity of illness. The nine or more hours of programming should be tailored to the individual and not be the same for every patient. This LOC should also have access to medications for addiction and psychiatric illness via telemedicine or direct care.
Level 2.5 Partial Hospitalization
This LOC can be done in the same setting as a level 2.1 but will need to provide at least 20 hours of programmed clinical intervention per week. This should be a mixture of individual, group, or self-help therapy. A patient should be living in a sober-living facility, at home, or in a shelter to receive this care efficiently. Both levels 2.1 and 2.5 can be “co-occurring enhanced,” which means that they will handle all outpatient psychiatric needs in-house.
Example: A patient with OUD, who meets the intensive outpatient or partial hospitalization LOC, will need highly structured behavioral interventions delivered by qualified personnel. Someone could simultaneously qualify for comprehensive level 1 care (an opioid treatment program) and still need level 2.1 or 2.5. The reason for this is that they would need both enhanced medical and medication monitoring as well as increased behavioral services.
Level 3.1, 3.5, and 3.7 (Residential)
Level 3.1 Clinically Managed Low-Intensity Residential Services
Level 3.1 is the first residential LOC and is designed for people who have little or no community connection, a high-risk living environment, or very low recovery skills. It is generally staffed by allied health professionals, peers, and group living workers. This is the least intensive level of residential treatment when it comes to direct services delivered.
Level 3.5 Clinically Managed High-Intensity Residential Services
This LOC is designed for patients with relationships that are abusive, chaotic, or non-supportive; who have not developed adequate coping skills for recovery; and who are in imminent danger, needing 24-hour stabilization and treatment. This LOC is staffed with licensed clinical staff, including social workers, licensed professional counselors, and addiction counselors. There are daily programmed services that should include cognitive behavioral therapies, motivational enhancement therapies, and psychotherapies. This LOC should have access to medications for addiction treatment and toxicological studies for monitoring purposes. They do not have to be on-site. There should be ongoing interdisciplinary assessments and treatment directed at inhibitors of recovery and linking to ongoing addiction treatment.
Level 3.7 Medically Monitored Intensive Inpatient Services
Level 3.7 includes physician monitoring and around-the-clock nursing care. This LOC includes access to psychiatric, toxicological, and lab services on-site, via referral or through telemedicine. This LOC is designed for patients with concerns in dimensions 1–3 (withdrawal, medical, and psychological) and the need for medical monitoring for these. There is direct delivery of clinical services as in Level 3.5.
While all of the levels described so far are considered “residential”, they vary based on the level of clinician oversite (the managing clinician may be an LCSW or a psychologist, etc.). Level 3.1 has the lowest need for clinical intervention and is generally not staffed with licensed clinicians and thus does not deliver psychotherapy. Level 3.5 provides the safety of a therapeutic environment and delivers behavioral therapies from licensed clinicians. The need for a patient to enter treatment in a specific level of care in a residential environment to go to residential can vary based on the stability of their living environment, their readiness to change, and their risk of relapse. For those with medical conditions that need medical monitoring, level 3.7 provides for 24-hour nursing care and access to an on-call physician.
Level 4.0 Medically Managed Intensive Inpatient Services (Hospital-Based Services)
Level 4.0 is a hospital LOC that includes addiction treatment. The care is managed by a physician who is responsible for diagnosis, treatment planning, and treatment. This care generally focuses on the withdrawal syndrome, stabilization of medical issues, or acute psychosis, but does not include direct addiction treatment by addiction counselors or clinicians.
A critical component to successful management of the chronic disease of addiction is that the LOCs should not live in isolated silos. Patients should be able to flow from one LOC to the other as their condition improves or worsens. This focus on patient response to treatment can be accomplished by community coordination of services through a central assessment and coordination location, contracted step-down pathways, and knowledge of the array of services delivered at each location. While this integrated system may seem like the idealized state, addiction medicine physicians and allied professionals have understood this need for over 30 years—now is the time to build the right components to deliver the right service at the right time. Importantly, patients with chronic pain may require special consideration throughout this continuum of care. In addition to treating SUDs, clinicians will need to work with these patients to adequately manage their chronic pain and their expectations of living with pain, which may require supplementary psychosocial supports.
Capacity: Where Most Patients Fall on the Continuum of Care
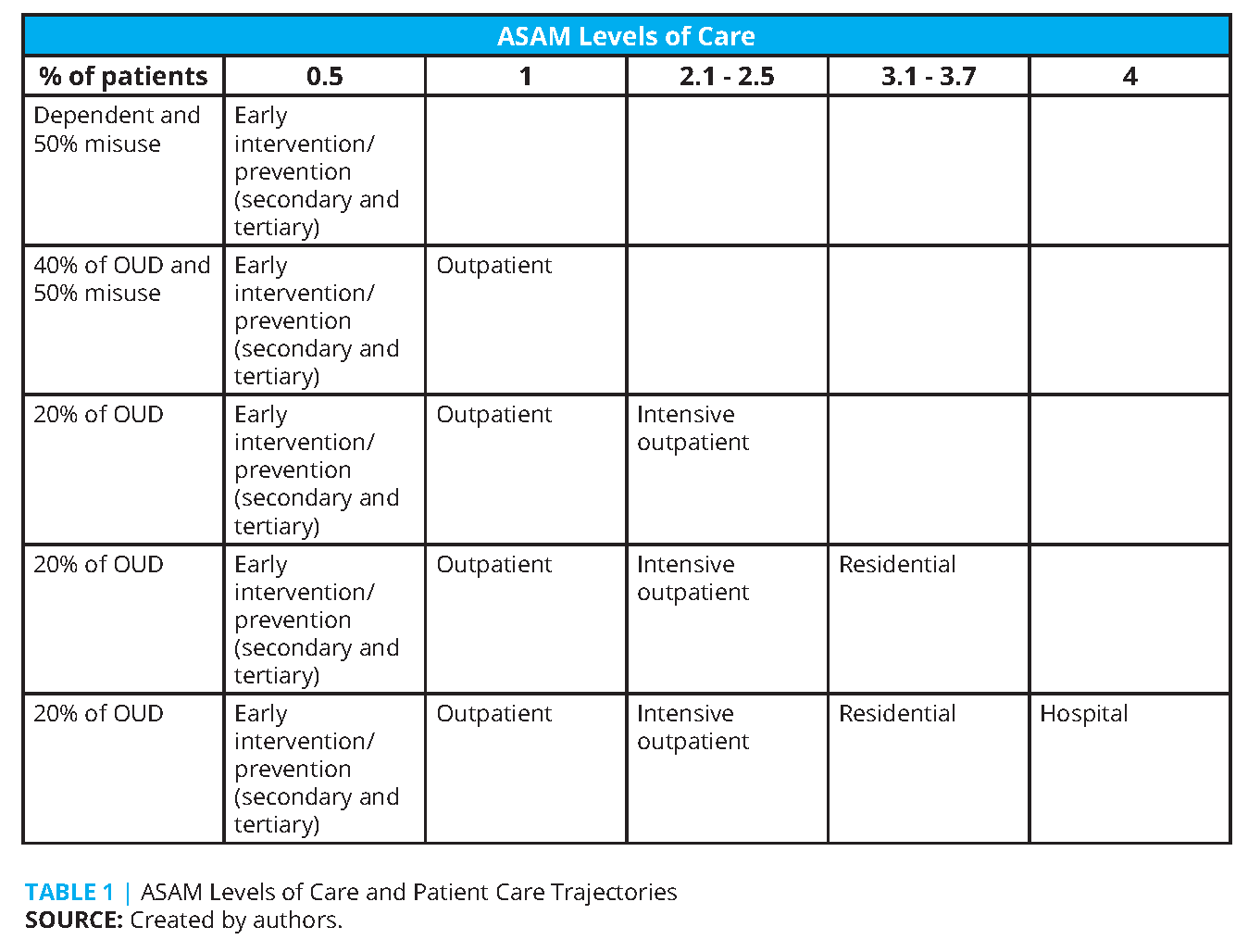
Because addiction is a chronic relapsing and remitting disease, the needs of patients may fluctuate, meaning they may need higher and lower LOCs over time. Therefore, the entire continuum of care must be considered for a patient’s course of treatment. It should be anticipated that patients could require higher LOCs as their disease worsens. A process that is more responsive to the needs of patients could consider the case of patients who begin care according to Table 1. For example, patients who suffer from mild OUD may begin and stay at level 1 outpatient, while others may need initial placement in level 4 treatment. Once stable in level 4, they will progress down the intensity cascade until in recovery. However, most patients do not progress in a linear fashion and will need restabilization after relapse. Experts and data from the ASAM Continuum evaluation tool estimate that 40-50 percent of OUD patients will start in level 1, while approximately 20 percent will need level 4 treatment.
The SUD treatment system in the U.S. does not conform to this ideal state, and treatment availability across the care continuum varies across the country. Data from internal ASAM surveys reveal that some experts feel that capacity is lacking in certain LOCs (e.g., intensive inpatient and outpatient) and have excess capacity for others (e.g., inpatient rehabilitation programs in level 3.5). However, this perception may be due to differing access to insurance, the array of services available, and the heterogeneity of quality throughout the continuum. Accessibility to all LOCs throughout the continuum is required for both clinical and cost-effective care to occur.
It is important for the ASAM Criteria to be used regardless of the actual substance(s) a person has been misusing. If a community or health plan does not have a full continuum of care available to treat people addicted to opioids, they most likely do not have the appropriate resources to treat people addicted to alcohol or methamphetamine. This leads to mismatched care and patients who feel lack trust in their care and providers and the system as a whole.
Capacity: Medication for Opioid Use Disorder (MOUD)
The use of MOUD is a core component of the management of OUD. Medical science shows that ongoing medication management saves lives, and the use of MOUD treatment is the gold standard of care [32]. Short-term medication use for withdrawal management is applied extensively in medically managed or medically supervised withdrawal management programs (ASAM levels 4 and 3.7). MOUD as a long-term maintenance treatment is most often associated with level 1 outpatient care. In an ideal state, MOUD with all three FDA-approved medications for OUD (methadone, buprenorphine, and extended-release naltrexone) would be a core treatment component throughout the entire residential and outpatient continuum of care [4]. If applied properly, the use of MOUD negates the need for inpatient withdrawal management.
The regulations surrounding each of these medications create different barriers for people seeking treatment. Methadone, the longest-standing MOUD, is initially dispensed daily at an independent OTP. This daily dosing can be helpful for those needing a stabilizing pattern of enhanced medication monitoring while minimizing disruptions to the responsibilities of daily life. However, for some patients who do not need this oversight, it is burdensome, expensive, and unnecessary. In contrast, oral buprenorphine has the ability to be dispensed frequently and flexibly at a pharmacy; however, currently, only practitioners who obtain a specialized DEA waiver can prescribe this medication [20], and they can only prescribe to a limited number of patients. Only 4 percent of doctors nationwide are waivered to prescribe buprenorphine and only half of those are active prescribers [21]. Given the limited availability and increased flexibility of oral buprenorphine treatment options in comparison to those of methadone, it is particularly concerning that Black patients are less likely than white patients to be prescribed buprenorphine. This disparity persists across income level, with wealthier individuals being more likely than lower-income individuals to have access to buprenorphine, and urgently needs to be addressed [70].
Naltrexone injections (extended-release Naltrexone) are administered monthly at a doctor’s office or clinic. As the least-regulated medication, extended-release Naltrexone requires abstinence (i.e., free from short- or long-acting opioids for 6 or 7–10 days, respectively, based on ASAM’s National Practice Guideline [6]) upon injection. The current rigid and asynchronous regulations for MOUD are not conducive to a well-functioning treatment system and frustrate an already complex problem. Having these medications fragmented across providers is antithetical to confronting OUD with personalized treatment options.
Another barrier to receiving MOUD is the administrative restrictions often faced by patients and physicians, including restrictive formularies, prior authorization, and step therapy or “fail first” protocols. If a patient is stable on a specific medication or formulation of the MOUD, but the medication is not on a health plan, Medicaid, or pharmacy benefit management company formulary, the patient may be forced to discontinue or delay therapy until a prior authorization can be completed. Sometimes, the prior authorization may be further delayed or denied altogether, forcing the patient into withdrawal or subjecting the patient to unaffordable costs for out-of-pocket payments to remain in compliance. According to a 2018 Substance Abuse and Mental Health Services (SAMHSA) report, only 42 state Medicaid programs reimburse for methadone for the treatment of OUD [45]. Patients may also face these hurdles if they switch insurance plans—in that one company might cover a particular formulation, but if that is not the formulation being used by the patient, the only way to obtain coverage may be for the patient to fail on the covered medication first. These policies are not evidence-based and can have deadly consequences. These issues are complicated even further by the fact that these policies diff er from state to state, making education surrounding prescribing complex at best and near impossible at worst.
For patients and providers who are able to navigate the fragmented medication system and a myriad of administrative barriers, patient outcomes have consistently proven that MOUD saves lives, prevents infectious disease, and provides economic benefits to patients and their communities. Methadone treatment is the most studied of the three of the FDA-approved medications and shows consistent retention in treatment—from 60 percent to as high as 80 percent over six months [23]. It is difficult to differentiate whether this is specifically a medication effect or the effect of being in a highly observed and consistent environment with daily interaction with treatment staff.
Studies show limited public support for the use of federal dollars for any form of addiction treatment [10], and only 19 percent of Americans endorse the use of methadone [31]—one of the most commonly used forms of MOUD [28]. As a result, many people do not seek treatment out of fear of being marginalized, especially by their coworkers and neighbors. Furthermore, one in seven rural providers will not prescribe buprenorphine because of issues with DEA intrusion into their practice [8].
While the results are very positive for a certain segment of patients, methadone maintenance can have limitations:
- The administration of methadone medication is highly regulated, limiting the number of treatment centers qualified to administer this form of treatment (special licenses and intense oversight required).
- Methadone treatment is typically delivered in an OTP daily, with each dose delivered to the patient under observed conditions, thus limiting this form of treatment for patients for which daily treatment is not a viable option. Only after a patient has been stable for six weeks will some states even allow patients to have take-home doses. For some, achieving “stability” can take years.
- Methadone treatment is associated with significant stigma.
- Methadone treatment clinics are not available in all geographic areas, and rarely in rural areas.
- Despite having the best outcomes for some patients, methadone still possesses the highest level of stigma of the MOUD treatment medications.
- Lack of insurance coverage contributes to access barriers for this treatment.
Capacity: Workforce Needed
The implementation of MOUD has not kept up with the growth of the opioid overdose epidemic in the U.S. The number of OTP clinics increased by only 36 percent from 2003 to 2016, and those offering buprenorphine treatment increased from 11 percent to 58 percent [3]. In the same timeframe, opioid-related overdose increased by approximately 230 percent [33]. In 2018, 20 percent of people with OUD received specialty addiction treatment [27]. To close this treatment gap, clinics need to be properly funded and administrated. However, the most beautiful building and the best administration cannot treat addiction without the appropriate workforce. The compensation structures that make this investment overly complicated are explored in detail below. The staffing numbers listed below take into account current limitations placed on providers by state and federal licensing. They are not endorsed by these authors, as they lack nuance and have little to no data to support them. However, they do represent the current state of the addiction medicine workforce.
Multiple barriers restrict the availability of top-of-the-line OUD treatment, including stigmatizing attitudes toward MOUD, cost of treatment for the individual, and restrictive regulations for prescribing [46]. One factor blocking access to appropriate treatment is the severe shortage of trained professionals available to meet the dramatically expanded treatment need dictated by the opioid overdose epidemic.
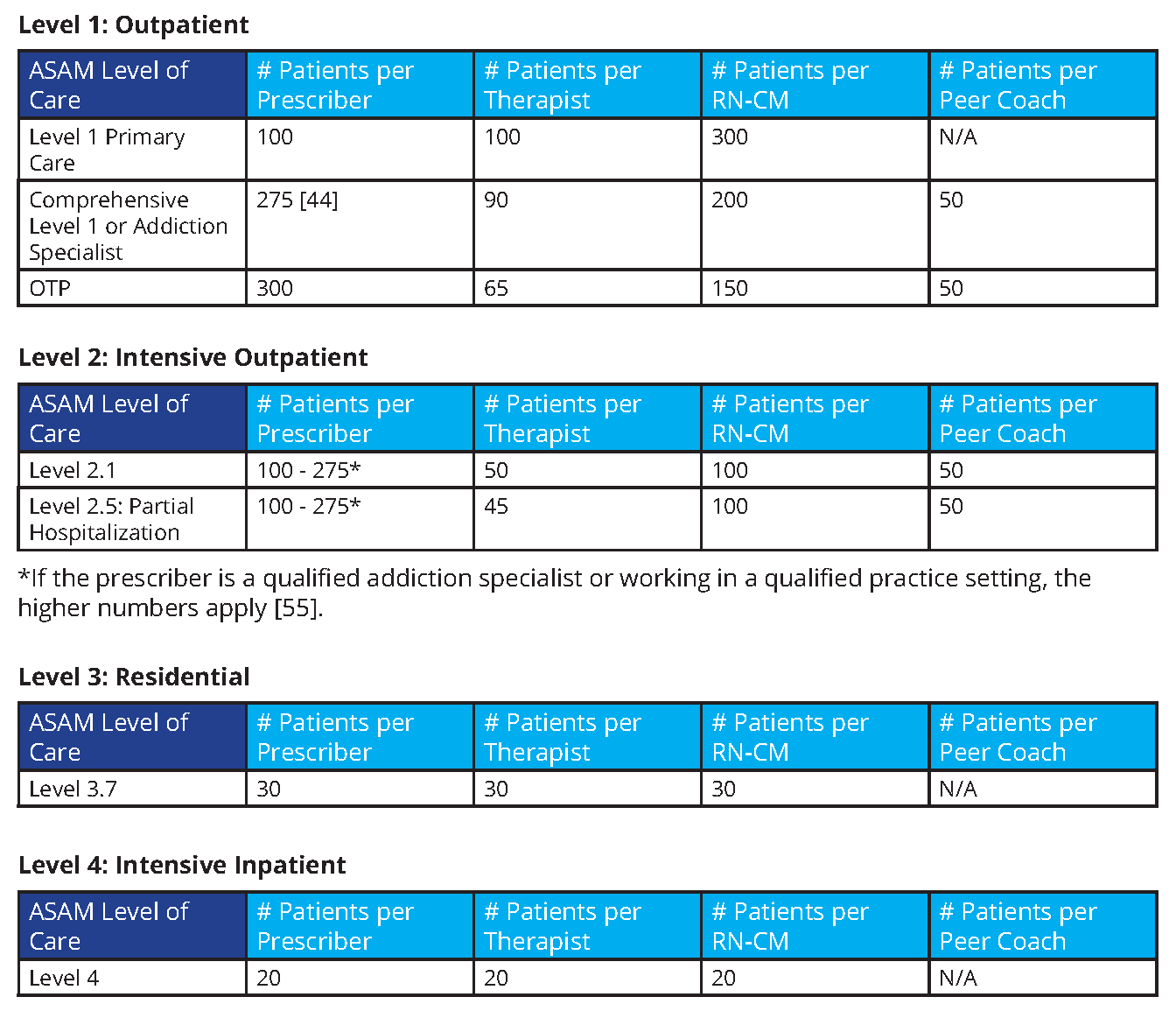
The schematics on the following page are examples of provider staffing needs at each ASAM LOC. The numbers in the schematic are derived from limits set forth by a combination of the DEA, state licensing boards, and current payment support mechanisms. Advanced practice clinicians, such as physician assistants and nurse practitioners, can only prescribe buprenorphine to 100 patients. Physicians can likewise only prescribe for 100 patients, increasing to 275 only if they are specialists or working within specific qualified practice settings. The numbers attributed to a therapist and case manager (CM) are restricted by scheduling capacity and, in some states, licensing limits. Peer limits are practical limitations as described by multiple peer-based interventions and presumes that peer support specialists are supportive of maintenance medications.
It is possible to extrapolate the appropriately-sized workforce needed for a town of 100,000 residents using the numbers outlined above. This scenario will build on the assumption that 10 percent of the population either has a SUD or suffers from misuse and requires an intervention. This estimation is much higher in communities that are hit hardest by the opioid crisis.
This extrapolation yields approximately 10,000 people needing care. To make this value more realistic, for the sake of this thought exercise, assume only 70 percent of those want help. This results in 7,000 people needing care, including differing levels of need and medications for OUD and SUD. Using the numbers in the schematic, this town of 100,000 would need approximately:
- 3 addiction specialists (covering an OTP, level 3.7 and level 4)
- 10 prescribers seeing 100 patients, or 50 prescribers seeing 20 patients
- 100 therapists
- 70 case managers
- 100 peers
For comparison, the current national average of psychiatrists per 100,000 is 12.9; the average number of addiction psychiatrists and addiction medicine physician specialists is 0.3 per 100,000 [56]. While this thought exercise is oversimplified, this example illustrates we only have a fraction of the staffing needs required for quality care. . This thought exercise also does not include those tasked with community supports for the myriad of social determinants of health or reentry needs. Given the need for multiple LOCs in the setting of a limited number of specialists, the addiction specialists we do have, are often stretched relatively thin compared to their specialty provider counterparts. Remember, in this example we are only talking about a city the size of San Angelo, TX—imagine the workforce needed in a city with over one million people. There is clearly a massive national effort needed to build an appropriately sized workforce, while leveraging the use of available technology to make the relatively small size of the current workforce operate more efficiently.
Capacity: Telehealth
Telehealth has been shown to be an effective modality to provide care for many medical and behavioral health conditions [2]. Despite the evidence for the appropriate and effective use of telehealth in certain conditions, telehealth uptake has generally been slow, largely because of the limitations in payment models and other regulatory barriers. With the onset of the COVID-19 pandemic and subsequent rollout of stay-at-home orders, telehealth rapidly emerged as the solution to provide care while avoiding potential COVID-19 transmission. Most notable has been the rapid expansion of telehealth by Medicare members. For example, in a six-week period, there was an 11,617 percent increase in Medicare member visits alone [36]. This increase was the result of a massive expansion of telehealth flexibilities at the federal level. Concurrently, one by one, states adopted their own flexibilities and updated regulations for the use of virtual platforms to deliver care. Along with the new payment allowances, additional flexibilities were announced that allowed the prescription of controlled substances via telehealth for both new and established patients, as well as the ability to use a broader array of technology platforms to communicate with patients. Finally, the DEA and SAMHSA put in place numerous flexibilities specifically for patients being treated with MOUD, including the ability to prescribe buprenorphine based on an audio-only telephone visit with a patient [74].
The change from in-person to virtual care is a paradigm shift in health care on the scale of the transition from paper charts to electronic health records (EHRs). In the case of EHRs, when federal funding was allocated to support this transition, there was rapid uptake by health systems. However, providers received little to no training to prepare and develop best practices. As a result of this lack of preparation and despite the potential benefits of EHRs, providers and patients alike have expressed widespread dissatisfaction with the system. Transitioning to virtual care is equally rapid and transformative to health care. The lessons learned from the EHR transition are applicable to help build the capacity to treat complex conditions like addiction in a virtual setting. For most providers, virtual care was not a choice but a necessity as COVID-19 spread across the country. Similar to the experience during the rapid expansion of EHRs, health teams are working to optimize telehealth as they are being forced to use it, and there are no clear best practices for virtual care in many settings. Making the transition to telehealth for addiction
care as effective as possible will require a focus on:
- clinician skill building and competency,
- development of accepted criteria on when to use virtual versus in-person modalities, and
- payment parity for virtual and in-person care.
Many providers and health systems have undergone meaningful practice transformation to a model of robust team-based care leading to improved engagement across the care team and optimization of each staff member’s unique role. As care teams move into the virtual clinical model, practices need to continue focusing on the role of each team member and their interaction with the patient. This can be challenging in a virtual environment when care is asynchronous and spread across locations. Practices need to resist returning to the provider/prescriber-centric model, a common occurrence when practices transitioned from paper to EHR. This is another opportunity to learn from past experiences as practices move through this paradigm shift.
Using telehealth to treat addiction and behavioral health conditions has several distinctly different approaches compared to addressing other physical or medical conditions. Most of these differences are related to the need to build an empathetic and responsive connection with the patient. Building such a connection is already difficult in the office setting, and physical separation only makes this more difficult. Although there may be less reliance on the “hands-on” physical examination (PE), there is a greater need to connect on a personal level that may be challenging in a virtual world. The clinician must be cognizant of addressing issues like unanticipated interruptions in connectivity and having distracting sounds in the background. Having standard tools and protocols to support this activity is a must. A broad set of skills are needed to treat a patient with addiction that requires mastery in a virtual environment including but not limited to:
- assessing the medical and behavioral condition of the patient and associated comorbidities;
- assessing other patient needs such as living situation, housing, family dynamics, and relationships; and
- assessing patient safety in real-time.
In response to physical distancing guidelines implemented during the COVID-19 pandemic, the DEA waived the requirement for an in-person visit prior to beginning buprenorphine treatment [37]. Many payers expanded their telehealth reimbursement to include additional services and increased payment to equal in-person visits. Each state has its own telehealth statutes and regulations that add to the variability in capacity for treatment.
One aspect of addiction treatment that is often overlooked are disparities associated with socioeconomic status. This equates to some patients having decreased broadband access, no data plans for their smartphone, and unreliable Wi-Fi connections. There is also a digital literacy divide that will need to be addressed for this population. While data is still being developed in how to effectively address these issues, the digital and literacy divide will continue to persist and cause gaps in care and treatment if not addressed in an expedited manner. However, some of these issues may be partially offset by the deceased need for travel, childcare, and absence from work that an in-person visit requires.
Capacity: Naloxone Education and Distribution
Naloxone is a medication that will reverse an opioid overdose. Naloxone is made available in the community for use in emergencies by multiple distribution methods, including co-prescription with opioids, standing state orders by public health physicians, and distribution through treatment programs and harm reduction programs such as syringe service locations (needle exchanges). Naloxone is also available in many areas as part of emergency medical kits and carried by first responders. These prescriptions can be provided for patients with a known OUD or those who take opioids for pain. Some states have expanded access to naloxone by allowing pharmacies to have a standing order for the medication, permitting anyone to receive the medication over the counter [57]. Forms of naloxone include intramuscular injection, nasal spray, and intravenous administration. Naloxone has saved tens of
thousands of individuals from death due to an opioid-related overdose.
Rapid and substantial expansion of naloxone distribution programs, including standing orders in pharmacies, has proven to save lives and reduce hospitalizations related to opioid overdose. The FDA has issued guidance to accelerate the development of over-the-counter naloxone, which could substantially expand access to this life-saving medication [41].
Naloxone distribution is most effective when strategically and equitably distributed to at-risk groups. This equates with free and low barrier availability at many locations. There are key distribution points that must be included in a naloxone allocation system for maximum harm reduction. These locations include:
- syringe exchange programs
- correctional departments, prisons, and jails
- housing shelters
- hospitals
- emergency departments
- community-based pharmacies
- community-based naloxone distribution programs
- health departments
- mobile health clinics
- safety net providers
- first responders, including law enforcement
The workforce capacity to distribute naloxone is often inadequate at the local level and often based on the opioid overdose rate in a community. Typically, full-time employees are required to run a publicly funded overdose education and naloxone distribution program, with support from other state agencies including the department of public health.
Capacity: Other Harm Reduction Services
Another key capacity-based strategy for addressing the opioid overdose epidemic is harm reduction programs like syringe services programs (SSPs). Harm reduction refers to any program that provides services to protect people who use drugs from disease or harm without demanding people to stop using substances. SSPs are community-based programs that provide access to free sterile needles and syringes and safely destroy used needles and syringes. These locations can also act as entry points for treatment, education, and care coordination. High-risk injection behaviors are strongly associated with several communicable diseases such as HIV and Hepatitis C. These and similar programs reduce the spread of disease while teaching safe injection practices and training individuals on overdose rescue [9]. Harm reduction strategies are highly stigmatized and often mischaracterized as enabling drug use. There is no proven association between the use of SSPs and increased drug use.
Besides the humanitarian argument to protect people in all stages of use and recovery from devastating infection, SSPs are economically advantageous. Preventing the contraction and spread of communicable diseases costs significantly less than the downstream costs of infection and death [53]. Return on investment (ROI) for these efforts is as high as $7 for every dollar spent [19], demonstrating very efficient use of funding to protect health. This ROI, specifically, accounts for only the cost of avoiding having to pay for HIV treatment alone—the addition of other avoided costs including hepatitis C and other related issues will further increase the ROI of these programs.
Such programs often use counselors and peer support staff who help patients navigate their way into a treatment program. Research consistently demonstrates the effectiveness of unused syringe access in preventing infectious disease transmission and soft tissue infections while also supporting the overall “health and well-being of drug users through linkages to drug treatment, medical care, housing, [overdose prevention, insurance coverage,] and other vital social services.” [75] SSPs also “respect, value, and prioritize the human rights and dignity of people who use drugs” [75] while challenging drug-related stigma.
Competency
The Institute of Medicine (now the National Academy of Medicine) defined the core competencies of medicine in 2002, which include patient-centered care, interdisciplinary practice, evidence-based practice, quality improvement, and informatics [24]. These competencies have not fully penetrated into addiction medicine at scale. Integrating research and providing evidence-based care has proven challenging in the addiction treatment and recovery system, as many (if not most) addiction treatment centers do not offer evidencebased medical treatment [71]. It is also evident that the core competencies in all of medicine are lacking an understanding of how structural racism and discrimination impact every level of treatment.
The main reason for the lack of evidence-based care is that addiction treatment has historically been siloed from traditional office-based medical and psychiatric practice. When this separation is coupled with stigma, structural racism, and discrimination, it becomes a potent mix that permeates the very core of a trusting relationship between a patient and a provider. Without clear practice guidelines, various forms of traditional and experimental treatments have been able to thrive without scientific evidence on their safety or efficiency. Without a baseline quality metric, the addiction treatment system does not have adequate means to standardize and improve its quality. Some medical providers are working to integrate addiction treatment into established primary care and psychiatric practices and publish guidelines based on this work. Addiction medicine has recently become a recognized field within the National Board of Medical Specialties, which will not only provide a scalable specialized clinical and research workforce, but also build emphasis on addictive diseases into the medical school curriculum, into hospital staff training, and throughout the medical care system.
While these efforts are critical to opening new avenues for care, the deeper issue lies with how health practitioners and the broader public understand addiction as an illness. In the U.S., two ends of a spectrum often emerge as to how addiction develops and is maintained: as a chronic relapsing and remitting disease as understood by the medical and scientific communities, or as a hedonistic failure of people who just “can’t say no.”
Too often, addiction has been treated as a behavioral and moral failure rather than a medical condition with behavioral symptoms [34]. For decades, the U.S. has relied on behavioral interventions such as detoxification, incarceration, and other legal penalties—all of which fail to address the underlying causes of addiction. While these interventions may make sense if addiction were an issue of poor choices and moral failings, the lack of effectiveness of these methods is consistent with what is now known about the brain science of addiction as a chronic disease. As with any disease, health providers need to address the needs of each patient for biological, psychological, and social interventions.
Framing addiction as a behavioral problem has allowed for the expansion of short-term treatment models such as withdrawal management and residential treatment. These facilities provide a space to “break” physical dependence on opioids and introduce behavioral changes but are not effective for long-term recovery [43]. After one year, the failure rate of withdrawal management alone is 80 percent, and withdrawal management alone may actually increase the risk of future overdose [43]. While residential treatment is part of the care continuum, different facilities offer a huge variation in the treatment, and therefore results are variable [38]. For example, some residential treatment programs may or may not offer individual counseling or MOUD. Some even require patients who are stable on MOUD to discontinue use, putting the patient at even further risk of overdose and death. Therefore, every residential treatment facility must be analyzed individually, and persons in crisis do not often have the time or the mental capacity to do so. Recovery residences also face their own stigma from neighborhood and community organizations, often as a result of the perception that people with OUD will attract poverty and crime to the community [25].
Because of structural racism, incarceration affects racial minorities at significantly higher rates than their white peers and has been used as a tool to control certain types of substance use for decades [40]. The “war on drugs” created a pervasive mindset that aligned certain types of drug use and criminality [35]. Although many people with OUD interact with the criminal justice system, few receive any form of evidence-based treatment while incarcerated or otherwise justice-involved [13]. This method of controlling certain substances and the people who use them does not work and is both catastrophic and costly to those within the criminal justice system as well as their families and social groups. The mass incarceration of people with SUD has devastating effects on family structures, most notably children [53].
Overdose is the most common cause of death among the formerly incarcerated, with the month after release being the most dangerous [11]. Initiating and continuing MOUD in jails and prisons is a common-sense way to reduce mortality but is rarely done. Removing a patient’s medication for a chronic illness as they encounter the justice system is cruel and unbefitting of their right to health care [12]. Providing methadone or buprenorphine treatment, per a patient-centered decision-making model, has been shown to significantly lower overdose deaths in the months post-incarceration [58].
Addiction medicine has traditionally been viewed as being outside of mainstream medicine and rarely taught in medical school or residency, as well as in all health professions. Due in part to the criminalization and stigma of addiction, this separation has even been codified in the Code of Federal Regulations (42CFR Part 2) by segregating the addiction-related medical records of those in treatment from the rest of their medical records. Given that addiction medicine is so separate from traditional medicine, and that health care providers are not immune to the deep stigma of addictive disease, those who do not work explicitly in addiction have increasingly felt that the extent of their ability to help is to order a referral for the patient to speak to a psychologist or social worker [59]. Now that overdose is the number one cause of injury-related death in the U.S. and the number one cause of death for people under 50 [18], the medical system must reorient toward appropriate and adequate care for those with addiction.
The latest estimates show that very few primary care and OB/GYN offices in the U.S. actively screen for addiction on a regular basis [47]. To address this gap, medical practices need to add the education and EHR capability to consistently and predictably apply validated verbal screening and early intervention, in order to meet new United States Preventive Services Task Force recommendations [60]. One method to reach this goal would be for the top five EHR systems to build out appropriate screening tools, toolkits, and order-sets for primary care develop online learning modules to promote a high degree of fidelity and precision.
The provision of addiction medicine via telehealth has become the reality for many providers since the COVID-19 outbreak. As previously discussed, this method of health care delivery was not carefully contemplated or optimized before its widespread use became a necessity. Technological competency, in the various modalities of telehealth, is going to be its own requirement in the future of addiction medicine. By definition, telehealth encompasses several modalities including live or asynchronous video visits, audio phone only, econsult (peer-to-peer interprofessional consultations), e-visits, and virtual check-ins. Depending on the needs of the individual patient, the treatment plan could include care provided over any of these platforms—a decision the provider should base on the individual. The provider, rather than regulatory agencies, should decide on whether it’s possible, appropriate, or in the patient’s best interest to provide care in these ways. As the use of telehealth becomes more universally accepted, the provider needs to develop the competency of understanding the appropriate use of these virtual care platforms. Whether to offer telehealth or to require an in-person visit should be at the discretion of the treating provider, who remains ultimately responsible for the quality and appropriateness of care. Whether to engage in telehealth care remains the choice of the patient, and the totality of the treatment plan should be done through a patient-centered and shared decision-making process.
Achieving telehealth competency for addiction treatment includes the ability to weigh the need for information that can only be collected in person against the ability to provide care over a virtual platform that otherwise would not be available to the patient. This would be described as “better than nothing.” Does the telehealth visit meet that standard? It should be the responsibility of the telehealth provider to decide whether it is in the best interest of the patient. The provider needs to consider factors of privacy and security, health care literacy and language skills, and the need for a PE or lab tests to complete the evaluation [61]. Deciding whether the need to treat or prescribe via telehealth outweighs the need for a PE and lab tests requires telehealth competency—and practicing without this competency puts the patient, the provider, and the virtual model of care each at their own varying risk.
Under the umbrella of telehealth or virtual care, econsult can be an effective way to provide the support of an addiction specialist to a patient’s care team. The value of e-consult is multidimensional: supporting the care provided by the primary provider, keeping more care in the medical home, developing the learning curve of primary providers, and avoiding gaps in care or drop offs as patients are lost in the referral system. Competency in the use of e-consult for addiction treatment is required for both the referring (primary provider) and the receiving or consultant provider. Similar to the traditional referral process, providers need to understand how to request appropriate referrals and how to ask for and give clinical recommendations in a virtual setting.
Another technology-based platform to increase competency and capacity is Project ECHO [49]. Although not technically telehealth, Project ECHO uses a virtual grand rounds-style model to “move knowledge, not patients.” The model, which started for support of primary care physicians caring for hepatitis patients across New Mexico, has grown to hundreds of Project ECHO virtual clinics across the U.S. and abroad, addressing a multitude of medical and behavioral health conditions, including SUD and addiction. Project ECHO is an excellent model to support primary care physicians as it meets many of the same goals of the e-consult, but in a virtual learning community setting, also allowing for virtual collaboration in a multidisciplinary learning community. The model includes education mixed with case-based presentations and discussions. Over time, primary care providers and their practices develop the skills and confidence to manage more conditions in the medical or behavioral health home. Both e-consult and Project ECHO support the competencies of providers to screen, diagnose, and treat patients with addiction.
Because of the current state of heterogeneous approaches to care, different levels of knowledge throughout addiction treatment, and a lack of the application of evidence-based medicine, the competency within every LOC that treats patients with addiction must be analyzed, addressed, and grown. Whether a physician or other prescriber, social worker, nurse, peer, or administrator, those treating patients with addiction should possess a baseline set of competencies that allows for a streamlined and evidence-based approach to care for every person entering treatment. Each of the individuals mentioned above must have sufficient education covering an array of topics. The
depth of knowledge for each of these topics is dependent on the location of service delivery, their profession, and the specialty of the provider delivering the service as well as their state’s delineation of their legal scope of practice. The following list of suggested competencies for those treating addiction in any setting is by no means exhaustive but aligns with published addiction medicine and addiction psychiatry competencies.
Structure of Addiction Interventions
- use of the ASAM Criteria
- outpatient approaches to care
- telehealth approaches to care
- residential approaches to care
- hospital-based approaches to care
Team-based Care
- components of high functioning teams [62]
- care implementation
- payment structures
Array of Services
- biomedical services (MOUD, infectious disease, etc.)
- co-occurring enhanced services
- pain evaluation and treatment
- withdrawal management
- housing
- case management, including consideration of the social determinants of health
- behavioral therapy services
Competencies for prescribers and healthcare professional staff supporting them (RNs, MAs, etc.) [63]
- prevalence and demography of addiction
- neuroscience and pathophysiology of SUDs
- motivational interviewing
- toxicological evaluation of SUDs
- assessment, PE, and diagnosis of SUDs and other addictions
- medications used for the treatment of SUDs
- recognition and treatment of withdrawal from substances
- effect of stigma and structural racism in treatment
- approaches to special populations with addiction (patients with chronic pain, pregnancy, etc.)
- the addiction treatment system
Competencies for therapists (psychologists, LCSWs, etc.) [64]
- prevalence and demography of addiction
- the six dimensions of the ASAM assessment
- psychiatric screening and assessment tools
- motivational interviewing
- evidence-based behavioral treatments for SUDs and other addictions
- adverse childhood experiences (ACEs) and their correlation with behavior
- effect of stigma and structural racism in treatment
- benefits of medications for addiction treatment
- social determinants of health and how they relate to addiction treatment
Competencies for counselors and behavioral health support staff (alcohol and other drug counselors, BSWs, etc.) [64]
- prevalence and demography of addiction
- screening and brief assessment of SUDs and other addictions
- psychiatric screening and assessment tools
- motivational interviewing
- evidence-based behavioral treatments for SUDs and other addictions
- ACEs and their correlation with behavior
- effect of stigma and structural racism in treatment
- benefits of medications for addiction treatment
- social determinants of health and how they relate to addiction treatment
Competencies for care coordinators [65]
- prevalence and demography of addiction
- screening and brief assessment of SUDs and other addictions
- motivational interviewing
- documentation and utilization management
- effect of stigma and structural racism in treatment
Competencies for peer support [66]
- building caring and collaborative relationships
- how to share lived experience
- how to provide support
- how to support recovery planning
- motivational interviewing
- crisis mitigation
- how to communicate with empathy
Reaching the competency of care that patients with addiction desire and deserve is a necessary and urgent task. Special consideration should be given to patients who require chronic pain management in addition to SUD treatment, which will require systematic incorporation of additional competencies related to pain management [69].
Consistency
The ideal treatment system sets up providers to provide high-quality care and ensures that standards are being met across the systems for patients with all types of medical conditions, including addiction. This consistent LOC also sets up a patient with addiction for success. Consistency is the predictable execution of knowledge and the correct application of evidencebased care in addiction treatment. While the ASAM Criteria help provide a tailored treatment plan and location of care for the patient, the medical care provided must adhere to best treatment practices. Consistency is measurable and can be observed in clinical decisions and patient outcomes across different domains. Currently, the Commission on Accreditation of Rehabilitation Facilities (CARF) and the Joint Commission accredit programs for a range of LOCs, but these do not currently confirm essential elements of consistent quality of care. ASAM and CARF have launched a joint voluntary certification program where level 3 programs for adults can receive external certification if their policies and procedures have the minimal core elements of ASAM levels 3.1, 3.5, and 3.7. The Joint Commission is also including ASAM LOC elements into some of its accreditation programs, and ASAM and the National Quality Forum (NQF) provide guidance on ways to measure quality consistently with their standards and performance measures [7]. While it is outside of this paper’s scope to present a detailed list and explanation of current performance and outcome measures, examples of some of these measures include:
- percent of patients prescribed medication for alcohol use disorder,
- percent of patients prescribed MOUD,
- all-cause inpatient residential readmission rate,
- presence of screening for a psychiatric disorder, and
- percent of patients followed up within seven days after withdrawal management episode.
To make these measures and measure concepts operational, it is important to aggregate and present them in a way that is consumable by key stakeholders. Measurement approaches also need to be able to capture variation in quality across the system.
While professional designations and certifications go a long way in upholding a standard of care, these approaches will not, on their own, advance the consistency of high-quality practice across the addiction treatment field. Too often these certifications are limited to specific LOCs, service types, and audiences and require opting in. To address this gap, the measurement paradigm needs to encourage and be transparent about the use of best practices by all addiction treatment facilities and include strategies to care for patients with the added need of chronic pain management. Such a paradigm needs to measure the use of best practices through a combination of validated data sources and public reporting. The measurement paradigm could triangulate quality measures by examining the structures, processes, and outcomes of a facility using a voluntary treatment facility survey, a crowd-sourced approach to patient experience feedback, and measures calculated using health insurance claims. An accessible website can be built to empower patients and their loved ones to navigate to the most appropriate, high-quality care. A website would also be accessible not just to people with OUD and their families while allowing state agencies, health insurers, and employers to align policies and payment decisions with the use of expert-agreed upon best practices. Although this is not a total solution, given lack of predictable access to internet and devices, it is a start and will allow for a much more transparent treatment system to exist.
A productive element of a measurement paradigm would be to voluntarily submit data which can then be centrally analyzed with benchmarking feedback given to the programs. In addition, initiatives for quality improvement in treatment settings should be data-driven in design against process metrics initially, growing into outcome metrics after core treatment quality processes are ensured. One measurement framework that encompasses these elements includes the nonprofit Shatterproof’s ATLAS (Addiction Treatment Locator, Analysis, and Standards Tool) framework [42]. Despite the promise of ASAM, NQF, and Shatterproof’s work, barriers to measuring quality may still persist. Eventually, all providers will need to provide transparent reporting on performance, quality, and outcome measures. Starting with benchmarking and incentives will go a long way to building a high reliability system of
care.
Compensation
Adequate funding is necessary for the delivery of services for people with addiction. As previously discussed, addiction services are often siloed from the payment and delivery of traditional medical services and mental health services. Addiction treatment and recovery services are often developed through a social service model outside of medical care—a model for payment and service delivery at odds with helping people manage what is recognized as a chronic brain disease. The current system of payment for addiction services in the U.S. marginalizes people with addiction, is unpredictable, and does not follow the mechanisms and evidence-based requirements in place for other medical treatment. Moreover, a streamlined process is needed to ensure adequate compensation of services for patients in need of both addiction care and chronic pain management.
It is important to recognize that while all health care issues are intimately tied with social determinants of health, it is inappropriate to focus on those issues without also ensuring a robust treatment system and recovery resources. Combating stigma and discrimination requires that compensation systems be put into place to allow care for people with addictive disease at the same level as for those with other conditions.
Compensation: Parity
The federal MHPAEA of 2008 required that some health insurance plans for mental health and addiction services have no less restrictive qualitative or quantitative limits than their coverage of other medical conditions [16]. This was a landmark law that applied to many health plans but still left many insured people without this protection. A range of other federal and state laws have added to these protections, often simply called “parity.” But these protections are only as good as their enforcement—and there is no robust enforcement of these parity requirements.
The concept of parity brings into stark relief the deficiencies of the current addiction treatment system. Typically, health plans would not pay for health care services that do not adhere to basic quality standards, such as the ability to prescribe medications to manage their condition. Yet the majority of addiction treatment programs in the country fail this basic test, while simultaneously receiving payment often from federal or state grants. “Parity” does not apply to those funding sources.
Compensation: Value-Based Payments and Fee Structures
Many health care organizations have been working to develop and implement alternative payment models that link payment to the ongoing management of chronic conditions or episodes of care as well as improvements in patient health outcomes instead of fragmented payments for each face-to-face encounter. Patient-centered medical homes and behavioral health integration are models that may be applicable to addiction treatment, but there are also some models that are specifically designed to improve patient health outcomes in addiction medicine. Examples include the Vermont Hub and Spoke model [72], the Virginia Medicaid Addiction and Recovery and Treatment Services (ARTS) model (see case example in Box 1), and the Patient-Centered Opioid Addiction Treatment model [73]. In addition, Medicare began paying for office-based OUD treatment with monthly bundled payments and for OTP services with weekly bundled payments in 2020.
Fundamental to value-based payment adoption is the requirement for consistency and clarity around the services being provided. Each state licenses programs and facilities with differing requirements, making it impossible for payers who manage benefits to truly compare the value of programs across state lines. Further, because there is currently no standardized external evaluation of the clinical care capacity of programs, payers and patients have no way to determine the actual treatment elements in place. This lack of consistency and transparency must be addressed for value-based payment structures to progress. Currently, CARF has an ASAM LOC certification program through which it certifies programs that meet the specific criteria of the LOCs described above. This type of certification, coupled with recent lawsuits that health plans must use national placement payment criteria for parity
compliance [48], has the potential to set the groundwork for improving quality and decreasing cost.
The ability to gather data on each patient’s journey through the health care system can be achieved by embedding a standardized high level of addiction-related data capture into EHRs. Doing this will not only allow for the EHRs to collect and report data that can be tied to payment but can also allow for measurement of the consistency in services provided. Pay-for-performance programs are predicated on incentivizing providers to get better outcomes for less cost without avoiding quality standards. The initial Health Maintenance Organizations of the 1980s often failed because they skimped on providing needed services to save money in the short term while setting patients up for harm and increased costs at a later date. Holding providers receiving payment to baseline quality standards, which is done currently throughout medicine, is noticeably absent in addiction treatment.
Payment dictates capacity over time. Whether fee-for-service or a value-based payment structure, if the payment for services is inadequate, an inadequate capacity will develop. If payment is provided for legacy care, which is not evidence-based or consistent with the standard of medical practice, such substandard care will proliferate in defiance of the underlying spirit of parity or stated wish to eliminate stigma and discrimination. Payment structures must be sufficient to support the delivery of medically appropriate care. The argument from payers that “there is no capacity for good care, so we have to pay for whatever is out there” would be challenged if the disease in question were cancer or diabetes rather than addiction. A promising case example is that of Virginia Addiction and Recovery Treatment Services (ARTS), which expanded addiction treatment coverage in line with Medicaid expansion, focused on alignment with the ASAM Levels of Care [50].
Compensation: Grant Funding
Much of the addiction care system is funded by federal and state grants, rather than traditional health plans such as Medicaid and Medicaid Managed Care Organizations. This process puts funding into an unsustainable process dependent upon annual appropriations and places it outside the usual medical quality assurance requirements and processes that are in place for other medical conditions. For example, Medicaid and Managed Medicaid provide data based on services received with claims on each individual, but a December 2020 U.S. Government Accountability Office (GAO) analysis of SAMHSA Substance Abuse Prevention and Treatment Block Grant Programs stated that the data on individuals served by these programs are unreliable [67].
The U.S. has attempted to impact the overdose crisis by allocating billions of new dollars to treat addiction and, in particular, for opioid addiction systems through the State Targeted Response to the Opioid Crisis Grants and State Opioid Response grants. The GAO revealed that states had significant difficulty in spending the grant funds that were available to them [67]. Multiple states had not accessed half of the funding available to them within one month of the end of the 24-month grant period, and most states faced challenges in fully spending the monies made available.
Issues identified as barriers to spending existing grants included lengthy contracting processes because of state rules, implementation delays, and surprisingly, provider reluctance to participate. Officials from multiple states indicated that some providers and local jurisdictions were reluctant to accept grant funding because they could not ensure the funding would continue after two years of hiring additional personnel, as well as reluctance to provide maintenance medication treatment such as buprenorphine [32]. Insufficient treatment capacity was ubiquitously identified as a main barrier to spending hundreds of millions of dollars of grant funds, particularly in rural areas, and the shortage of treatment professionals such as physicians and licensed social workers trained in addiction was noted as especially lacking.
Given that the grant programs noted above represent some of the most significant recent federal funding approaches to address the opioid crisis, it is critical to understand the lessons learned from those efforts to date. Simply allocating additional funding via grant programs into the current educational and legacy treatment programs has not led to a decrease in overdose deaths. Further attempts to fund care—before funding universities and other training programs for providers and before funding quality oversight mechanisms to ensure the treatment available is appropriate—can be expected to deliver the same impacts in the near term.
Compensation: Telehealth
The biggest hurdle of large-scale uptake of telehealth services for addiction treatment has been compensation because of reimbursement barriers. During the COVID-19 public health emergency, CMS announced significant Medicare flexibilities for providing virtual care to lessen the regulatory burden, keep patients at home, and decrease transmission of COVID-19. In doing so, the practice of medicine was not only permitted under Medicare, but encouraged, to be offered via telehealth. For many providers, virtual visits were one of the few sources of revenue to replace the drastic decrease in revenue from the loss of in-person care.
Now that some of these compensation barriers have become more flexible in light of the COVID-19 pandemic, it is critically important to meet the standard of care and avoid situations of potential fraud, waste, or abuse of the newly allowed flexibilities. Particular to the treatment of addiction has been the need to prescribe MOUD using telehealth. Previous to COVID-19, this practice was restricted and limited due to DEA regulations for prescribing controlled substances via telehealth—most notably the Ryan Haight Act’s in-person exam requirement. The SUPPORT ACT (Public Law No: 115-271) mandated the DEA to make the overdue clarifications and process for a special registration to engage in the practice of telemedicine. This issue remained unresolved at the time of the onset of COVID-19 and the new telehealth flexibilities by the DEA overrode the Ryan Haight Act. In doing so, several key changes emerged, including the ability to prescribe controlled medications via telemedicine for a new patient not already in established care and via audio-only initiation with respect to buprenorphine for the treatment of OUD. These unprecedented circumstances could be built on to avoid gaps in care and gaps in prescription coverage during a time of particularly high risk of overdose.
Compensation: State Medicaid Coverage
One of the most important considerations to ensuring appropriate compensation is the availability of Medicaid in individual states or other supporting health insurance to cover people with addiction. As the U.S. entered into the opioid overdose epidemic, the states that had expanded Medicaid under the provisions of the Affordable Care Act had a head start over non-expansion states on covering medication for MOUD and addiction treatment services. Without this expansion to cover the cost of treatment, patient outcomes are significantly worse. As the opioid overdose epidemic is changing to one driven by illicit fentanyl, methamphetamine, and cocaine, it will be essential to ensure that all SUDs can be addressed, which will undeniably put further strain on the system to provide adequate care.
Simple supply and demand can be applied to this problem—if there is an inadequate supply of evidence-based care, one way to alleviate the problem is to increase the compensation for that care. In the case of Medicaid and Medicare payments, there are other structural impediments, including:
- use of fee schedules that do not reimburse for needed services (physicians and providers cannot be reimbursed if there is a primary care provider visit and an addiction specialist visit on the same day);
- low reimbursement rates that require volume-driven care;
- low rates, which lead to very thin margins, limiting expansion and quality improvement by providers;
- access barriers such as prior authorizations for medications to treat addiction;
- grants versus sustainable funding development for SUD treatment programs;
- lack of technical assistance support to assist grant-funded legacy providers in the evolution to evidence-based care with billable services and financial stability; and
- lack of requirements to provide standard of care in order to receive payments.
It is often noted that, particularly in behavioral health, “health care coverage does not equal health care access.” While that can hold true, adequate payment is a critical step to increase access to evidence-based treatment for addiction.
Compensation: Commercial Plans
The need to ensure value in health care services has led to the management of health care benefits by most employer-sponsored plans, Medicaid, and many federal health care purchasers. Lack of enforcement of the range of parity laws and regulations has allowed continued discrimination in the coverage of mental health and addiction conditions. The ramification of this is well known within human resources departments across the U.S., where behavioral health conditions remain a significant source of absenteeism, workers compensation, and disability issues. Access to behavioral health services, including addiction treatment, is often challenging because of a series of factors including in-network provider availability (and specialization in the case of SUD), insurance coverage, and stigma.
Payment change must precede (or at least coincide with) quality and capacity improvement to adequately fund sustainable improvements. While payment rates from commercial plans are typically higher than Medicaid, low rates by these payers contribute to inadequate access to quality care. The following list highlights specific commercial plan coverage challenges that must be addressed.
- High payments: Extremely high payments are processed for out-of-network and out-of-state low-quality providers. Continuing to pay providers who provide care that is not only unhelpful but actively harmful diverts resources from ensuring the availability of quality care and leads to increased attitudes that “treatment doesn’t work.”
- Human resources departments: Those engaged in benefit systems to employee assistance plans and interfacing with direct supervisors should be approach addiction in the same manner as other medical conditions [68].
- Network adequacy: These issues include the availability of a sufficient number of qualified in-network providers who are accepting new patients, the wait time for appointments, the distance and travel time (geographic access coverage) to these providers’ offices, and telemedicine service access for the individuals covered by the plan.
- Total cost of care: Payers should be held accountable to gather and maintain a total cost of care and total quality of care for individual employees. Siloed data between behavioral health, medical, lab, and imaging claims for patients is problematic to understanding the true cost of medical care. An overemphasis on decreasing a behavioral health cost to the business purchasing the health plan may lead to underestimation of the additional related medical costs (e.g., when a person who is not receiving appropriate addiction treatment has a motor vehicle accident with resultant major medical expenses). Accurate data for patients and dependents can
drive greater access to and use of more valuable addiction care. - Parity laws: Working with state departments of insurance, the US Department of Labor, and other responsible agencies’ state attorneys general to conduct and meaningfully enforce state and federal mental health and SUD parity laws. This includes requiring health insurance companies and behavioral health management organizations to demonstrate compliance at the time of rate and form filing. Because parity laws are comparative by design, comparative analyses should be provided before plans are approved to be marketed and sold to consumers.
- Expansion: People across the U.S. continue to be devastated by the effects of drug use, ill-informed drug policies, addiction, and overdose—particularly Black, Latinx, Native American, and other traditionally marginalized communities. New payment structures need to take into account these issues and create culturally informed approaches.
Priorities for Ensuring Accountability and Transparency in Addiction Treatment
The resources available to support addiction care will always be finite, but significant improvements can be made. The U.S. addiction care delivery system was not built upon the understanding of addiction as a chronic medical condition and can hardly be described as a “system” at all. It has largely been funded outside the medical system, and therefore lacks the quality requirements in place for other types of medicine. The time for transparency and accountability has come. Building capacity, competency, and consistency requires leadership in the compensation quarter. The following priorities, while not exhaustive, list fundamental areas to be addressed to move the U.S. into an effective and efficient system of care.
- Identify and ensure availability of the entire continuum of care as defined by state and national guidelines and the capacity priorities outlined in this manuscript. (capacity)
- Ensure qualified providers can bill for treatment of addiction by eliminating the coverage chasm in which a behavioral health plan will only reimburse psychiatrists or board-certified addiction specialists to treat OUD, and the medical plan will not pay for treatment of OUD. All hands must be on deck to treat addiction comprehensively. (capacity, competency, and compensation)
- Shift funding incentives to programs that meet baseline quality standards and demonstrate positive outcomes. Increasing payment for quality treatment that meets baseline care standards will be necessary for those programs to develop and grow. (consistency and compensation)
- Eliminate the barriers of information exchange. Incentivize EHR data capture. Incentivize payers to integrate claims data for individuals across the range of carve-outs including behavioral health, medical, pharmacy, and laboratory. (competency, consistency, and compensation)
- Standardize care delivery levels and ensure compliance with requirements. Standardize LOCs by licensing and contracting treatment programs by national criteria such as the ASAM Criteria. Require oversight of programs via an independent evaluation of clinical care quality including state on-site inspections, CARF’s ASAM LOC certification, or other means. (consistency)
- Enforce current parity laws and regulations. Currently, parity or MHPAEA, is without significant enforcement action. While the specific nature of proposed enforcement legislation is beyond the scope of this report, all federal and state parity rules require attention and active enforcement. (compensation)
- Find and eliminate instances of fraud and predatory practices that have arisen as a result of poor enforcement of quality standards—for example, “phantom networks” where health plans identify that they have sufficient addiction providers, but when a patient calls them, these alleged providers will not see them. Secret-shopper programs should be used to identify the extent of plan phantom networks, with substantial penalties for the plans that contain them. (compensation)
Prioritizing these areas and considering the full range of the addiction treatment system will help to move the U.S. into a paradigm where we treat addiction as the chronic relapsing disease that it is and ensure that those with addiction have access to comprehensive, durable, high-quality, and evidence-based treatment.
Join the conversation!
![]() Tweet this! Authors of a new #NAMPerspectives discussion paper call for a long-term, sustainable approach to preventing and managing addiction as a chronic disease. Read about their proposed framework: https://doi.org/10.31478/202104b #OpioidCollaborative
Tweet this! Authors of a new #NAMPerspectives discussion paper call for a long-term, sustainable approach to preventing and managing addiction as a chronic disease. Read about their proposed framework: https://doi.org/10.31478/202104b #OpioidCollaborative
![]() Tweet this! “Policymakers and health leaders have an opportunity to make targeted investments dedicated to repairing the damage done by the drug overdose epidemic and preventing further harm.” Read about a proposed approach: https://doi.org/10.31478/202104b #OpioidCollaborative
Tweet this! “Policymakers and health leaders have an opportunity to make targeted investments dedicated to repairing the damage done by the drug overdose epidemic and preventing further harm.” Read about a proposed approach: https://doi.org/10.31478/202104b #OpioidCollaborative
![]() Tweet this! To adequately respond to America’s multifactorial drug overdose and death epidemic, the ecosystem in which people with addiction receive treatment must be reimagined and made more robust. Read about a proposed approach: https://doi.org/10.31478/202104b #OpioidCollaborative
Tweet this! To adequately respond to America’s multifactorial drug overdose and death epidemic, the ecosystem in which people with addiction receive treatment must be reimagined and made more robust. Read about a proposed approach: https://doi.org/10.31478/202104b #OpioidCollaborative
Download the graphics below and share them on social media!
References
- Adams, J. M. 2020. Making the Case for Syringe Services Programs. Public Health Reports 135(1_suppl):10S-12S. https://doi.org/10.1177/0033354920936233
- Totten, A. M., R. N. Hansen, J. Wagner, L. Stillman, I. Ivlev, C. Davis-O’Reilly, C. Towle, J. M. Erickson, D. Erten-Lyons, R. Fu, J. Fann, J. B. Babigumira, K. J. Palm-Cruz, M. Avery, and M. S. McDonagh. 2019. Telehealth for Acute and Chronic Care Consultations. Comparative Effectiveness Review No. 216. (Prepared by Pacific Northwest Evidence-based Practice Center under Contract No. 290-2015-00009-I.) Agency for Healthcare Research and Quality.
https://doi.org/10.23970/AHRQEPCCER216 - Alderks, C. E. 2017. Trends in the Use of Methadone, Buprenorphine, and Extended-Release Naltrexone at Substance Abuse Treatment Facilities: 2003-2015 (Update). CBHSQ Report: Substance Abuse and Mental Health Services Administration. Available at: https://www.ncbi.nlm.nih.gov/books/NBK469748/ (accessed January 27, 2021).
- American Society of Addiction Medicine Continuum. 2015. What are the ASAM Levels of Care? Available at: https://www.asamcontinuum.org/knowledgebase/what-are-the-asam-levels-of-care/ (accessed January 27, 2021).
- American Society of Addiction Medicine. n.d. What is The ASAM Criteria? Available at: https://www.asam.org/asam-criteria/about (accessed January 27, 2021).
- American Society of Addiction Medicine. 2020. The ASAM National Practice Guideline for the Treatment of Opioid Use Disorder—2020 Focused Update. Available at: https://www.asam.org/Quality-Science/quality/2020-national-practice-guideline (accessed January 27, 2021).
- American Society of Addiction Medicine. n.d. Standards and Performance Measures. Available at: https://www.asam.org/Quality-Science/quality/standards-and-performance-measures (accessed January 27, 2021).
- Andrilla, C., C. Coulthard, and E. H. Larson. 2017. Barriers Rural Physicians Face Prescribing Buprenorphine for Opioid Use Disorder. Annals of Family Medicine 15(4):359-362. https://doi.org/10.1370/afm.2099
- Aspinall, E. J., D. Nambiar, D. J. Goldberg, M. Hickman, A. Weir, E. Van Velzen, N. Palmateer, J. S. Doyle, M. E. Hellard, and S. J. Hutchinson. 2014. Are needle and syringe programmes associated with a reduction in HIV transmission among people who inject drugs: a systematic review and meta-analysis. International Journal of Epidemiology 43(1):235-248. https://doi.org/10.1093/ije/dyt243
- Barry, C. L., E. E. McGinty, B. A. Pescosolido, and H. H. Goldman. 2014. Stigma, discrimination, treatment effectiveness, and policy: public views about drug addiction and mental illness. Psychiatric Services 65(10):1269-1272. https://doi.org/10.1176/appi.ps.201400140
- Binswanger, I. A., P. J. Blatchford, S. R. Mueller, and M. F. Stern. 2013. Mortality after prison release: opioid overdose and other causes of death, risk factors, and time trends from 1999 to 2009. Annals of Internal Medicine 159(9):592-600. https://doi.org/10.7326/0003-4819-159-9-201311050-00005
- Bone, C., L. Eysenbach, K. Bell, and D. T. Barry. 2018. Our Ethical Obligation to Treat Opioid Use Disorder in Prisons: A Patient and Physician’s Perspective. Journal of Law, Medicine, and Ethics 46(2):268-271. https://doi.org/10.1177/1073110518782933
- Boutwell, A. E., A. Nijhawan, N. Zaller, and J. D. Rich. 2007. Arrested on heroin: a national opportunity. Journal of Opioid Management 3(6):328-332. https://doi.org/10.5055/jom.2007.0021
- Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration, US Department of Health and Human Services. 2020. Results from the 2019 National Survey on Drug Use and Health: Graphics from the Key Findings Report. Presentation. Available at: https://www.samhsa.gov/data/sites/default/files/reports/rpt29393/2019NSDUHFFRBriefSlides082120.pdf (accessed January 27, 2021).
- National Center for Health Statistics. n.d. Provisional Drug Overdose Death Counts. Available at: https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm (accessed January 27, 2021).
- Centers for Medicare and Medicaid Services. n.d. The Mental Health Parity and Addiction Equity Act (MHPAEA). Available at: https://www.cms.gov/CCIIO/Programs-and-Initiatives/Other-Insurance-Protections/mhpaea_factsheet (accessed January 27, 2021).
- Chen, Q., M. R. Larochelle, D. T. Weaver, A. P. Lietz, P. P. Mueller, S. Mercaldo, S. E. Wakeman, K. A. Freedberg, T. J. Raphel, A. B. Knudsen, P. V. Pandharipande, and J. Chhatwal. 2019. Prevention of Prescription Opioid Misuse and Projected Overdose Deaths in the United States. JAMA Network Open 2(2):e187621. https://doi.org/10.1001/jamanetworkopen.2018.7621
- Drug Policy Alliance. n.d. Drug Overdose. Available at: https://drugpolicy.org/issues/drug-overdose (accessed January 27, 2021).
- Nguyen, T. Q., B. W. Weir, D. C. Des Jarlais, S. D. Pinkerton, and D. R. Holtgrave. 2014. Syringe exchange in the United States: a national level economic evaluation of hypothetical increases in investment. AIDS and Behavior 18(11): 2144-2155. https://doi.org/10.1007/s10461-014-0789-9
- Bliley, T. 2000. Drug Addiction Treatment Act of 2000. H.R. 2634 Jul 27, 2000. Available at: https://www.congress.gov/bill/106th-congress/house-bill/2634/actions (accessed January 27, 2021).
- George, J. 2018. Why Do So Few Docs Have Buprenorphine Waivers? MedPage Today, February 14. Available at: https://www.medpagetoday.com/psychiatry/addictions/71169 (accessed January 27, 2021).
- Haffajee, R. L., L. A. Lin, A. S. B. Bohnert, and J. E. Goldstick. 2019. Characteristics of US Counties With High Opioid Overdose Mortality and Low Capacity to Deliver Medications for Opioid Use Disorder. JAMA Network Open 2(6):e196373. https://doi.org/10.1001/jamanetworkopen.2019.6373
- Hser, Y. I., A. J. Saxon, D. Huang, A. Hasson, C. Thomas, M. Hillhouse, P. Jacobs, C. Teruya, P. McLaughlin, K. Wiest, A. Cohen, and W. Ling. 2014. Treatment retention among patients randomized to buprenorphine/naloxone compared to methadone in a multi-site trial. Addiction 109(1):79-87. https://doi.org/10.1111/add.12333
- Institute of Medicine. 2003. Health Professions Education: A Bridge to Quality. Washington, DC: The National Academies Press. https://doi.org/10.17226/10681
- Kennedy-Hendricks, A., C. L. Barry, S. E. Gollust, M. E. Ensminger, M. S. Chisolm, and E. E. McGinty. 2017. Social stigma toward persons with prescription opioid use disorder: Associations with public support for punitive and public health-oriented policies. Psychiatric Services 68(5):462-469. https://doi.org/10.1176/appi.ps.201600056
- Madras, B. K., N. J. Ahmad, J. Wen, J. Sharfstein, and the Prevention, Treatment, and Recovery Working Group of the Action Collaborative on Countering the US Opioid Epidemic. NAM Perspectives. Discussion Paper, Washington, DC. https://doi.org/10.31478/202004b
- McCance-Katz, E. F. 2018. SAMHSA/HHS: An Update on the Opioid Crisis. Presentation. Available at: https://www.samhsa.gov/sites/default/files/aatod_2018_final.pdf (accessed January 27, 2021).
- Substance Abuse and Mental Health Services Administration. 2019. 2019 National Survey of Drug Use and Health (NSDUH) Releases. Available at: https://www.samhsa.gov/data/release/2019-national-survey-drug-use-and-health-nsduh-releases (accessed January 27, 2021).
- US Senate. n.d. CONNECT for Health Act of 2019. Available at: https://www.schatz.senate.gov/imo/media/doc/CONNECT%20for%20Health%20Act%20of%202019%20(2).pdf (accessed January 27, 2021).
- US Senate. 2020. TREATS Act. Available at: https://www.congress.gov/bill/116th-congress/senatebill/4103 (accessed January 27, 2021).
- Moore, P. 2015. Poll Results: Heroin. YouGov, January 20. Available at: https://today.yougov.com/topics/politics/articles-reports/2015/01/20/pollresults-heroin (accessed January 27, 2021).
- National Academies of Sciences, Engineering, and Medicine. 2019. Medications for Opioid Use Disorder Save Lives. Washington, DC: The National Academies Press. https://doi.org/10.17226/25310
- National Institute on Drug Abuse. n.d. Overdose Death Rates. Available at: https://www.drugabuse.gov/drug-topics/trends-statistics/overdose-deathrates (accessed January 27, 2021).
- Peele, S. 1987. A moral vision of addiction: How people’s values determine whether they become and remain addicts. Journal of Drug Issues 17(2), 187-215. https://doi.org/10.1177/002204268701700205
- Pembleton, M. R. 2017. We’ve spent a century fighting the war on drugs. It helped create an opioid crisis. The Washington Post, August 31. Available at: https://www.washingtonpost.com/news/madeby-history/wp/2017/08/31/weve-spent-a-centuryfighting-the-war-on-drugs-it-helped-create-an-opioid-crisis/ (accessed January 27, 2021).
- Pifer, R. 2020. Medicare members using telehealth grew 120 times in early weeks of COVID-19 as regulations eased. Health Care Dive, May 27. Available at: https://www.healthcaredive.com/news/medicare-seniors-telehealth-covid-coronavirus-cmstrump/578685/ (accessed January 27, 2021).
- US Drug Enforcement Administration. 2020. Untitled Letter. Available at: https://www.deadiversion.usdoj.gov/GDP/(DEA-DC-022)(DEA068)%20DEA%20SAMHSA%20buprenorphine%20telemedicine%20%20(Final)%20+Esign.pdf (accessed January 27, 2021).
- Reif, S., P. George, L. Braude, R. H. Dougherty, A. S. Daniels, S. S. Ghose, and M. E. Delphin-Rittmon. 2014. Residential treatment for individuals with substance use disorders: assessing the evidence. Psychiatric Services 65(3):301-312. https://doi.org/10.1176/appi.ps.201300242
- Gramlich, J. 2020. Black imprisonment rate in the US has fallen by a third since 2006. Pew Research Center, May 6. Available at: https://www.pewresearch.org/fact-tank/2020/05/06/share-of-blackwhite-hispanic-americans-in-prison-2018-vs-2006/ (accessed January 27, 2021).
- Pew Trusts. 2018. More Imprisonment Does Not Reduce State Drug Problems. Available at: https://www.pewtrusts.org/en/research-and-analysis/issue-briefs/2018/03/more-imprisonment-does-notreduce-state-drug-problems (accessed January 27, 2021).
- Sharpless, N. E. 2019. Statement on continued efforts to increase availability of all forms of naloxone to help reduce opioid overdose deaths. US Food and Drug Administration, September 20. Available at: https://www.fda.gov/news-events/press-announcements/statement-continuedefforts-increase-availability-all-forms-naloxonehelp-reduce-opioid-overdose (accessed January 27, 2021).
- Shatterproof. n.d. ATLAS (Addiction Treatment Locator, Assessment, and Standards Platform). Available at: https://www.treatmentatlas.org/ (accessed January 27, 2021).
- Smyth, B. P., J. Barry, E. Keenan, and K. Ducray. 2010. Lapse and relapse following inpatient treatment of opiate dependence. Irish Medical Journal 103(6):176-179. Available at: https://pubmed.ncbi.nlm.nih.gov/20669601/ (accessed January 27, 2021).
- Substance Abuse and Mental Health Services Administration. n.d. Understanding the Final Rule for a Patient Limit of 275. Available at: https://www.samhsa.gov/sites/default/files/programs_campaigns/medication_assisted/understanding-patient-limit275.pdf (accessed January 27, 2021).
- Substance Abuse and Mental Health Services Administration. n.d. Medicaid Coverage of Medication-Assisted Treatment for Alcohol and Opioid Use Disorders and of Medication for the Reversal of Opioid Overdose. Available at: https://store.samhsa.gov/product/Medicaid-Coverage-of-Medication-Assisted-Treatment-for-Alcohol-and-Opioid-Use-Disorders-and-of-Medication-for-the-Reversal-of-Opioid-Overdose/SMA18-5093 (accessed January
27, 2021). - Substance Abuse and Mental Health Services Administration. n.d. Table of Contents for the 2018 NSDUH Detailed Tables. Available at: https://www.samhsa.gov/data/sites/default/files/cbhsq-reports/NSDUHDetailedTabs2018R2/NSDUHDetailedTabs-TOC2018.htm (accessed January 27, 2021).
- Svikis, D. S., and K. Reid-Quiñones. 2003. Screening and prevention of alcohol and drug use disorders in women. Obstetrics and Gynecology Clinics of North America 30(3):447-468. https://doi.org/10.1016/s0889-8545(03)00082-2
- Casetext. n.d. Wit v. United Behavioral Health. Available at: https://casetext.com/case/wit-v-united-behavioral-health-8 (accessed January 27, 2021).
- Project ECHO. n.d. Project ECHO. Available at: https://hsc.unm.edu/echo/ (accessed January 27, 2021).
- Virginia Commonwealth University. 2020. An Evaluation Report Prepared for the Virginia Department of Medical Assistance Services—Addiction and Recovery Treatment Services, Access and Utilization During the Second Year (April 2018–March 2019). Available at: https://hbp.vcu.edu/media/hbp-dev/pdfx27s/policy-briefs/arts/AddictionandRecoveryTreatment-Services_ACC.pdf (accessed January 27, 2021).
- US Centers for Disease Control and Prevention. 2001. HIV and AIDS—United States, 1981–2000. MMWR Weekly 50(21):430-434. Available at: https://www.cdc.gov/mmwR/preview/mmwrhtml/mm5021a2.htm (accessed January 27, 2021).
- Linas, B. P., A. Savinkina, C. Barbosa, P. P. Mueller, M. Cerdá, K. Keyes, and J. Chhatwal. 2021. A clash of epidemics: Impact of the COVID-19 pandemic response on opioid overdose. Journal of Substance Abuse Treatment 120:108158. https://doi.org/10.1016/j.jsat.2020.108158
- Blanco, C., M. M. Ali, A. Beswick, K. Drexler, C. Hoffman, C. M. Jones, T. R. A. Wiley, and A. Coukell. 2020. The American Opioid Epidemic in Special Populations: Five Examples. NAM Perspectives. Discussion Paper, National Academy of Medicine, Washington, DC. https://doi.org/10.31478/202010b
- American Society of Addiction Medicine. 2020. The ASAM National Practice Guideline for the Treatment of Opioid Use Disorder: 2020 Focused Update. Available at: https://www.asam.org/docs/defaultsource/quality-science/npg-jam-supplement.pdf?sfvrsn=a00a52c2_2 (accessed January 27, 2021).
- World Health Organization. 2009. Clinical Guidelines for Withdrawal Management and Treatment of Drug Dependence in Closed Settings. Geneva, Switzerland.
- Scutti, S. 2019. 21 million Americans suffer from addiction. Just 3,000 physicians are specially trained to treat them. Association of American Medical Colleges, December 18. Available at: https://www.aamc.org/news-insights/21-million-americans-suffer-addiction-just-3000-physicians-are-speciallytrained-treat-them (accessed January 27, 2021).
- Abouk, R., R. L. Pacula, and D. Powell. 2019. Association Between State Laws Facilitating Pharmacy Distribution of Naloxone and Risk of Fatal Overdose. JAMA Internal Medicine 179(6):805-811. https://doi.org/10.1001/jamainternmed.2019.0272
- JAMA Network. 2018. Examination of Postincarceration Fatal Overdoses After Addiction Treatment Medications in Correctional System. Available at: https://media.jamanetwork.com/news-item/examinationpostincarceration-
fatal-overdoses-addiction-treatment-medications-correctional-system/ (accessed January 27, 2021). - van Boekel, L. C., E. P. M. Brouwers, J. van Weeghel, and H. F. L. Garretsen. 2013. Stigma among health professionals towards patients with substance use disorders and its consequences for healthcare delivery: Systematic review. Drug and Alcohol Dependence 131(1-2):23-35. https://doi.org/10.1016/j.drugalcdep.2013.02.018
- US Preventive Services Task Force. 2020. Final Recommendation Statement—Unhealthy Drug Use: Screening. Available at: https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/drug-use-illicit-screening#fullrecommendationstart (accessed January 27, 2021).
- US Department of Veterans Affairs. n.d. CRE 12-010—HSR&D Study. Available at: https://www.hsrd.research.va.gov/research/abstracts.cfm?Project_ID=2141701898 (accessed January 27, 2021).
- Beaulieu-Volk, D. 2015. 7 qualities of high-functioning healthcare teams. Fierce Healthcare, April 10. Available at: https://www.fiercehealthcare.com/healthcare/7-qualities-high-functioning-healthcare-teams (accessed January 27, 2021).
- American Board of Addiction Medicine. n.d. Core Competencies for Addiction Medicine. Available at: https://www.abam.net/become-certified/corecompetencies/ (accessed January 27, 2021).
- Substance Abuse and Mental Health Services Administration. n.d. Addiction Counseling Competencies: The Knowledge, Skills, and Attitudes of Professional Practice. Available at: https://store.samhsa.gov/sites/default/files/d7/priv/sma12-4171.pdf (accessed January 27, 2021).
- Hoge, M. A., J. A. Morris, M. Laraia, A. Pomerantz, and T. Farley. 2014. Core Competencies for Integrated Behavioral Health and Primary Care. Washington, DC: SAMHSA-HRSA Center for Integrated Health Solutions. Available at: http://womenshealthcouncil.org/wp-content/uploads/2016/11/WF-Core-Competencies-for-Integrated-Behavioral-Health-and-Primary-Care.pdf (accessed January 27, 2021).
- Substance Abuse and Mental Health Services Administration. n.d. Core Competencies for Peer Workers in Behavioral Health Services. Available at: https://www.samhsa.gov/sites/default/files/programs_campaigns/brss_tacs/core-competencies_508_12_13_18.pdf (accessed January 27, 2021).
- US Government Accountability Office. 2020. Substance Use Disorder: Reliable Data Needed for Substance Abuse Prevention and Treatment Block Grant Program. Available at: https://www.gao.gov/assets/720/711215.pdf (accessed January 27, 2021).
- Kentuckiana Health Collaborative. n.d. Opioids and the Workplace: An Employer Toolkit for Supporting Prevention, Treatment, and Recovery. Available at: https://khcollaborative.org/member_resource/opioids-the-workplace/opioids-and-the-workplace/ (accessed January 27, 2021).
- Center for Substance Abuse Treatment. 2012. Managing Chronic Pain in Adults With or in Recovery from Substance Use Disorders. Rockville (MD): Substance Abuse and Mental Health Services Administration. Available at: https://pubmed.ncbi.nlm.nih.gov/22514862/ (accessed January 27, 2021).
- Lagisetty, P. A., R. Ross, A. Bohnert, M. Clay, and D. T. Maust. 2019. Buprenorphine Treatment Divide by Race/Ethnicity and Payment. JAMA Psychiatry 76(9):979-981. https://doi.org/10.1001/jamapsychiatry.2019.0876
- Jones, C. M., D. J. Byrd, T. J. Clarke, T. B. Campbell, C. Ohuoha, and E. F. McCance-Katz. 2019. Characteristics and current clinical practices of opioid treatment programs in the United States. Drug and Alcohol Dependency 205:107616. https://doi.org/10.1016/j.drugalcdep.2019.107616
- Brooklyn, J. R., and S. C. Sigmon. 2017. Vermont Hub-and-Spoke Model of Care for Opioid Use Disorder: Development, Implementation, and Impact. Journal of Addiction Medicine 11(4):286-292. https://doi.org/10.1097/ADM.0000000000000310
- American Society of Addiction Medicine. n.d. Patient-Centered Opioid Addiction Treatment (P-COAT): Alternative Payment Model (APM). Available at: https://www.asam.org/docs/default-source/advocacy/asam-ama-p-coat-final.pdf?sfvrsn=447041c2_2 (accessed January 27, 2021).
- U.S. Department of Health and Human Services. 2020. Telehealth: Delivering Care Safely During COVID-19. Available at: https://www.hhs.gov/coronavirus/telehealth/index.html (accessed March 19, 2021).
- National Harm Reduction Coalition. 2020. Guide to Developing and Managing Syringe Access Programs. Available at: https://harmreduction.org/issues/syringe-access/guide-to-managing-programs/ (accessed March 19, 2021).