Jason B. Gibbons
Samantha Murrell
Donna Kinzer
Joshua M. Sharfstein
Introduction
The United States has shown that higher health care spending does not guarantee better health outcomes. Despite consistently leading the world in health care spending per capita, U.S. population health outcomes are poor (Papanicolas et al., 2018). Compared to ten other high-income countries in the Organization for Economic Co-operation and Development (OECD), the U.S. has the lowest life expectancy, the most significant burden of chronic disease, and the highest rate of preventable deaths (The Commonwealth Fund, 2019). Furthermore, the accompanying growth in the utilization of patient cost-sharing mechanisms (e.g., high deductible health plans), significant treatment intensity associated with care delivery, and high unit prices for health care services have translated into a high prevalence of medical burden, with 100 million Americans (41% of adults) saddled with medical debt (Stephenson, 2022). There is a growing consensus that innovations in payment models and sustained investments in the social determinants of health (SDoH) are imperative for improving community health and health equity.
Community health is “the health status of a defined group of people and the actions and conditions, both private and public (governmental), to promote, protect, and preserve their health” (McKenzie et al., 2005). Many areas of the U.S. experience poor community health, exemplified by gaps in life expectancy of more than 20 years between neighborhoods within U.S. cities. Health equity is achieved when “everyone has a fair and just opportunity to be as healthy as possible. Attaining health equity requires addressing obstacles to health such as poverty, discrimination, and their consequences, including powerlessness and lack of access to good jobs with fair pay, quality education and housing, safe environments, and health care” (Braveman et al., 2017). The evolving COVID-19 pandemic has revealed the intersection of community health with health equity. Many communities experienced a lack of workplace protections, inadequate income, unsafe environments, and lack of access to needed health care, leading to profoundly inequitable outcomes, including mortality (Magesh et al., 2021; Samuel et al., 2021; Sze et al., 2020; Vasquez Reyes, 2020).
An essential dimension of both community health and health equity is racial justice. Many populations with poor health outcomes and inequitable access to health care services are also communities of color. These communities have also experienced centuries of discriminatory practices in health, education, employment, income, and criminal justice systems.
In recent years, there have been an increasing number of commitments from policy makers to advancing community health outcomes, health equity, and racial justice. New leadership at the Centers for Medicare & Medicaid Services (CMS) has embraced health equity as a strategic goal and has begun to orient payment models to its advancement (Seshami and Jacobs, 2022). The recently published CMS Innovation Center Strategy Refresh affirmed the advancement of health equity as a strategic objective. CMS has sought comments and ideas from a wide variety of stakeholders (CMS, 2021).
In the present paper, the authors propose an innovative payment model that realigns incentives across the necessary stakeholders, programs, and payments in metropolitan areas to advance community health and achieve health equity.
This paper is organized into a background section and a model proposal section. In the background section, we describe the relevance of existing and emerging payment systems to community health and health equity. In the model proposal section, we propose a global payment model with community health and health equity as its organizing features (hereafter, “the global equity model” or “GEM”). “Global” within this context refers to a form of cost control characterized by setting a cap on the totality of a health system’s revenue across inpatient, emergency department (ED), and outpatient sites of care.
Existing Reimbursement Frameworks and Their Relationship with Community Health and Health Equity
Introduction
Prevailing payment models have failed to address health equity issues directly while, in some cases, perpetuating distorted incentives that entrench and propagate health disparities. Recent payment innovations have shown promise and provide an important foundation for even more ambitious payment models that improve community health and equity as a fundamental objective.
Fee-for-Service
Still, the most widely used payment framework in the U.S., fee-for-service (FFS), is poorly aligned with good health outcomes (Zuvekas and Cohen, 2016). It incentivizes providers to deliver as many high-margin services as possible to maximize reimbursement (Zuvekas and Cohen, 2016). Consequently, inefficiencies result from waste and low-value care, which are disproportionately delivered to socially vulnerable (low socioeconomic status, uninsured, non-English speaking) and racially diverse populations (Schpero et al., 2017). There is generally little financial incentive for providing preventive and wellness services and even less for collaborations that address health equity. In FFS, as social vulnerability and disparities worsen health, the amount of low-value and wasteful services provided in the highest cost setting (i.e., acute care hospitals) increases, setting in motion a perverse set of incentives that increases revenue for health care providers and organizations while continuing to provide inadequate health care services to the population. Thus, FFS also incentivizes a de-investment in low-income communities and further exacerbates health disparities.
Alternative Payment Models
In response to the poor health outcomes associated with care delivery for the American people, policy makers and payers have sought to control costs and improve health by leveraging alternative payment models (APMs) to increase provider accountability for cost and outcomes (Nussbaum et al., 2018). Many APMs, however, do not have a strong track record of advancing health equity. APMs generally reward or penalize health care organizations based on the costs and outcomes for a set of attributed patients. Unfortunately, the accountability metrics for current APMs do not include health equity. Furthermore, the current mechanisms for determining patient attribution and reimbursement under many existing APMs have, in many cases, undermined organizations that serve populations burdened by health disparities. In the succeeding subsections, we briefly describe common APMs and their relationship to health equity.
Bundled Payments
There are two main types of bundled payment models: retrospective and prospective. Under the retrospective system, providers continue to bill under FFS but track their costs against a pre-determined benchmark (“target price”). Payers will reimburse providers up to the benchmark if they spend less than the target (Offodile et al., 2019). If providers exceed the target price, they become liable to payers for the overruns. Under the prospective payment model, payers make a single up-front payment for an entire episode of patient care. If providers spend more on the episode than they receive reimbursement for, they generate a financial loss (Offodile et al., 2019). Conversely, providers obtain savings if costs fall under budget.
In both models, quality metrics (e.g., risk-adjusted 30-day readmissions) serve as guardrails against the provision of inappropriate care. These design features of bundled payments create an incentive for providers to reduce spending while preserving quality. Associated clinical quality improvements can also help address health disparities while maintaining the incentives to reduce costs. At least one prominent bundled payment model, the Comprehensive Care for Joint Replacement (CJR) model, reduced the gap in hospital readmissions and post-acute care discharges between Black and White patients undergoing knee and hip replacement (Kim et al., 2020).
However, these models do not incentivize primary and secondary disease prevention and are inadequate for promoting health equity broadly. Even in the CJR model, overall outcome disparities remained in the program (Kim et al., 2021). Likewise, since the underlying payment mechanism is still rooted entirely in FFS, this model has limited opportunity to impact overall spending and redirect resources to health improvement.
Comprehensive Primary Care Model
The Comprehensive Primary Care Plus model is an APM that aims to strengthen the provision of primary care. In this model, practices receive a blended reimbursement that entails (1) a standard FFS payment component, (2) an incentive-based payment conditional on meeting clinical performance and patient experience targets, and (3) a quarterly payment per beneficiary per month. Unfortunately, meeting the program performance benchmarks and objectives required for reimbursement has been challenging for low-resourced and low-capacity practices (such as federally qualified health centers) that serve socially vulnerable communities, limiting their participation (Fraze et al., 2018). In general, payment models that use absolute performance targets effectively create high barriers to entry for practices in communities with high social risk, exacerbating the health equity divide. In addition, because primary care practices are often financially strapped, the potential to generate significant investments in prevention through these models alone is limited.
Traditional Accountable Care Organizations
In this model, provider networks called accountable care organizations (ACOs) assume responsibility for the totality of care for a set of attributed patients. Patients are attributed to ACOs if participating providers deliver a plurality of the evaluation and management services over a year. ACOs receive shared savings payments if they can successfully limit attributed patient spending below a benchmark while improving quality. Unfortunately, ACOs can sometimes “game” or circumvent the system by referring patients with substantial comorbidities to external non-ACO providers to avoid responsibility for their health and spending (Markovitz et al., 2019). To the extent that they can influence the attribution and reimbursement process, ACOs have little incentive to address health disparities. The ACO model can support more integrated care for patients. However, beneficiaries served by more extensive health care provider networks, including ACOs, are more likely to be White and have less social vulnerability (Anderson et al., 2014). Moreover, integration of care with social services has been demonstrably low among early ACO adopters due to a lack of data, limited partnerships with community-based organizations, and the absence of sustainable funding (Murray et al., 2020). Together, these factors could explain why ACO-attributed populations have less diversity than the general Medicare population (Lewis et al., 2017). There is also evidence that ACOs often form in areas characterized by fewer Black patients, lower uninsured rates, fewer patients from lower socioeconomic backgrounds, and fewer patients without advanced education. Correspondingly, ACOs with a high representation of minority patients have also been shown reproducibly to perform worse on quality metrics, indicating that traditional ACOs are inadequate to impact existing health disparities (Lewis et al., 2017; Yasaitis et al., 2016; Lewis et al., 2013).
The CMS ACO REACH Model
ACO REACH is a new APM that incorporates equity-based model elements. It refocuses previous benefit design, up-front payments, governance, data sharing, and provider selection to include additional consideration for equity. ACO reach also requires ACOs to create specific health equity plans. Health equity plans are roadmaps describing how ACOs will work to provide resources and services in underserved communities to reduce local health disparities in ACO catchment areas. ACO REACH also requires participating providers and at least two beneficiary advocates to serve on the board. Finally, ACO REACH will have greater oversight and vetting of model participants by CMS. Model participants include standard Medicare Shared Savings Program ACOs, new entrant ACOs (organizations that have not typically provided services to Medicare patients), and high-needs population ACOs (ACOs with a history of serving high-needs Medicare populations). Participating providers participate in one of two voluntary risk-sharing agreements: (1) the Professional with 50% shared savings/losses and a monthly risk-adjusted primary care capitation payment, and (2) the Global with 100% savings/losses having either a monthly risk-adjusted primary care capitation payment or a total care capitation payment for all covered services. The new ACO REACH model takes an essential step toward incorporating equity considerations into value-based payment. However, the equity design elements in this model are still not directly tied to cost and quality performance. Future payment reform is needed to ensure payment for equity improvement becomes a central component of APM.
Accountable Health Communities
In 2017, CMS introduced the Accountable Health Communities (AHC) Model. The idea was to expand the unit of risk to allow for community-level innovation and shared community resources to reduce health resource utilization and improve outcomes by providing screening services, navigation assistance, and community provider referrals to socially vulnerable Medicare and Medicaid beneficiaries. After its first three years, an evaluation showed the model to be associated with a 9% reduction in emergency room (ER) visits (CMS, 2020). Unfortunately, the program did not lead to net savings on medical expenditures and only fulfilled health-related social needs in 15% of cases (CMS, 2020). Still, the AHC provides evidence of the potential for future payment systems to become more oriented to non-medical causes of poor health.
Advancing Health Equity
Advancing Health Equity is a new initiative designed with equity as a central focus. This effort is a partnership between the Robert Wood Johnson Foundation, the Institute for Medicaid Innovation, the Center for Health Care Strategies, and the University of Chicago. The initiative works with Medicaid agencies, Medicaid managed care health plans, and health care organizations to help design value-based payment (VBP) models that support health care delivery transformations and incentivize the reduction of health and health care disparities (Patel et al., 2021). Learning collaboratives and strategic partnerships like Advancing Health Equity represent an important step to finding solutions to the current lack of equity-based incentives in health care payment models. However, it may prove challenging to achieve their goal of building upon the existing chassis of VBP models that have a long history of failing to improve health equity.
The CMS Health Equity Action Team
In response to recent calls for new APMs to focus on improving equity, CMS has created the Health Equity Advisory Team (HEAT) in collaboration with the Health Care Payment Learning & Action Network. HEAT focuses on benefit and payment redesign that rewards providers and health care organizations for addressing community SDoH that lead to health inequity. Its general mission is to empower private and public payers, providers, community organizations, and members of the community to identify causes of local health inequity and work together to create patient-centered and culturally appropriate interventions.
Risk Adjustment and Alternative Payment Models
Risk adjustment is a statistical process that updates quality performance and reimbursement based on specified attributes of the population. One purpose of risk adjustment is to ensure that hospitals and health clinics treating patients with complex medical and social needs are not unfairly penalized or rewarded because of the characteristics of the patients they serve. In recent years, there has been a vigorous debate over the use of risk adjustment for social factors in APMs (Joynt et al., 2017). Some have argued for risk adjustment because it allows for more fair competition and comparison between health care organizations. The argument is that those that take care of more populations experiencing more significant inequities but achieve comparable results deserve similar rewards. However, such an approach treats social risk factors as disease conditions rather than characterizing them as modifiable factors for the model itself.
For this reason, others argue against risk adjustment on the grounds that all health care organizations should be held to the same standards. This perspective reflects concern that risk adjustment efforts will lead to comprehensive efforts to assess risks (and thus improve reimbursement) but fewer incentives to reduce risks. However, the challenge remains that organizations serving communities with significant social risks often have worse health outcomes and fare more poorly in unadjusted models (Baker et al., 2021).
An alternative approach to the question of social risk adjustment is from the vantage point of community health and health equity. This perspective is underpinned by a central question: What is the best approach to addressing social drivers of poor community health? One method is to provide greater up-front and bonus payments to health care organizations that serve low-income communities and meet standard metrics (Jaffery and Safran, 2021). Another approach is to focus on community health outcomes and reward health care systems that make progress in reducing historical levels of illness and disease in their communities.
Global Payment Models
Global payment models aim to incentivize health care systems to improve the health of their communities. Under this paradigm, payers provide health systems with fixed payments to deliver care for a specified period to a predefined patient population, generally everyone in a clearly identified geographic area. These models reduce the reliance on service volume to drive revenue by making revenue more predictable. Moreover, emerging global health system payment models have demonstrated the potential to focus on core measures of community health at the population level (Murray, 2009).
Maryland’s Global Model
The evolution of hospital payment in Maryland is an example of how global models can be integrated into existing payment structures. Since the 1970s, Maryland has operated under an all-payer rate-setting system where the rates for individual services in each hospital are the same for all payers (i.e., Medicare, Medicaid, and commercial). A Medicare waiver in the Social Security Act exempted Maryland from the prospective payment systems that determined the rates of hospital care elsewhere in the country and allowed the state to set its rates (CMS, 2019; Murray, 2009). A global payment model was initiated in Maryland in 2014 through a shift in hospital payments from fixed rates to flexible rates that meet an annual all-payer budget amount that encompasses all care sites (inpatient, outpatient, ER).
The primary goals of the model were to improve the quality of care, measured by outcomes such as rates of 30-day hospital readmissions and potentially preventable complications, and control Medicare costs compared to national trends (CMS, 2019). The addition of the Care Redesign Program in 2017 provided optional pathways to improve the efficiency of hospital care and encourage collaboration between hospitals and community-based providers. The independent evaluation conducted for the Center for Medicare and Medicaid Innovation (CMMI) found savings for Medicare of nearly $1 billion in the model’s first four and one-half years (CMS, 2019). Likewise, there were accomplishments in reducing avoidable admissions. For example, admissions for ambulatory care-sensitive conditions decreased by 6.7% for Maryland Medicare beneficiaries and 6.1% for commercial plan members relative to comparison groups. Lastly, the differential effects of early global payment model implementation on vulnerable Medicare populations (dual eligibility, disabled, non-White, and rural) were recently examined (Masters et al., 2022). In sum, dual-eligible, disabled, and high comorbidity burden (i.e., multiple chronic conditions) beneficiaries were associated with greater reductions in acute care utilization and expenditures than their counterparts. This suggests that care redesign activities initiated in response to the Maryland global budget may have prioritized these high social need, high acute beneficiary populations.
Maryland transitioned to a Total Cost of Care (TCOC) model in 2019, through which Maryland committed to cost goals for inpatient and outpatient care (Matematica, 2021). This model’s inclusion of non-hospital providers and the addition of the Maryland Primary Care Program expanded on the progress of its predecessor (Matematica, 2021). Hospitals stand to benefit as preventable admissions in their catchment areas decline. As a result, they have the flexibility to reinvest savings under the global model rather than losing revenues under an FFS system. Furthermore, Maryland is using incentives in the TCOC model to focus on reducing the incidence of diabetes, overdose, maternal mortality, and childhood asthma at the population level.
In 2021, Maryland and CMMI added a Statewide Integrated Health Improvement Strategy to the TCOC Model, introducing targets for disparity reduction and other specified population health and outcomes targets.
Pennsylvania’s Global Model
In Pennsylvania’s Rural Health Model, launched in 2017, participating rural hospitals received a fixed budget to cover expenses from annual inpatient, ED, and outpatient services, with the expectation that they meet quality performance targets. The model’s objective is to provide rural hospitals with financial stability while simultaneously improving rural health care quality and community health metrics (CMMI, 2021b). A fundamental requirement of participation in the model is that each hospital establishes a Rural Hospital Transformation Plan. These plans detail how hospitals will work with local stakeholders and communities to enhance access to care and address population health. Several focus areas of the program include improved care coordination, medication management, palliative care, enhanced primary care, specialty care, and care management for chronic conditions, opioid use disorder treatment and overdose prevention, geriatric wellness, and weight management and healthy eating.
Vermont’s Global Model
The State of Vermont is in the fourth year of collaborating with the federal government to shift Medicare payment incentives from rewarding volume under a traditional FFS model to a single state ACO. Like Maryland’s All-Payer system, Vermont’s All-Payer Accountable Care Organization Model Agreement aims to reduce spending by emphasizing preventive care, more collaboration between providers, and investment in population health (CMMI, 2021b). Unlike Maryland, Vermont’s ACO model uses payer-specific benchmarks for attributed populations rather than an all-payer global payment. The main focus areas include decreasing chronic disease prevalence, lowering overdose and suicide rates, and increasing access to primary care. The model has made significant progress toward improving these areas and has also produced reductions in Medicare spending and improved the health of Vermont’s population, including the uninsured (CMMI, 2021a).
The Global Equity Model (GEM)
Introduction
U.S. communities that experience health care inequities generally account for a disproportionate share of health care costs; in these areas, the nation spends more, but residents are less healthy (Laveist et al., 2011). This dilemma reflects the high cost of the health and financial impacts of the SDoH as well as poor access to preventive and community-based services. When fragmented and inequitable care leads to excessive reliance on ERs and hospital clinics, fewer community resources are available to support preventive care, creating a vicious circle.
Therefore, the authors propose GEM, a payment framework focused on improving community health and health equity. The goal of the GEM is to reduce preventable illness and associated costs and use the savings to support attention to upstream social drivers of health, creating a virtuous circle.
This section provides an overview of the GEM concept. GEM should be implemented in areas experiencing substantial inequities in health (“health equity regions”). Eligible areas should be geographically contiguous and characterized by the following criteria: (1) a high concentration of health disparities relative to state or national levels (e.g., lower life expectancy, higher maternal mortality, higher incidence of diabetes) and (2) area-level economic deprivation. These areas are likely to be characterized by high per capita costs to the Medicare program due to high levels of preventable hospitalization (Khullar et al., 2020). This geographic location might include a single county, an amalgamation of counties, or a collection of zip codes. The key is that the geography is of sufficient size, scope, and relevancy to serve as a market for health systems.
In this region, the GEM should (1) reorganize payments for health systems through global payments, (2) incorporate a robust primary care model, (3) engage and empower the community through a health transformation plan and shared governance, and (4) be accountable to meaningful outcome metrics (see Figure 1). Under this framework, the success or failure of the health care system should be determined by measures of increasing health and health equity—the health of populations served, reductions in health care disparities, and creation of opportunities for health and well-being.
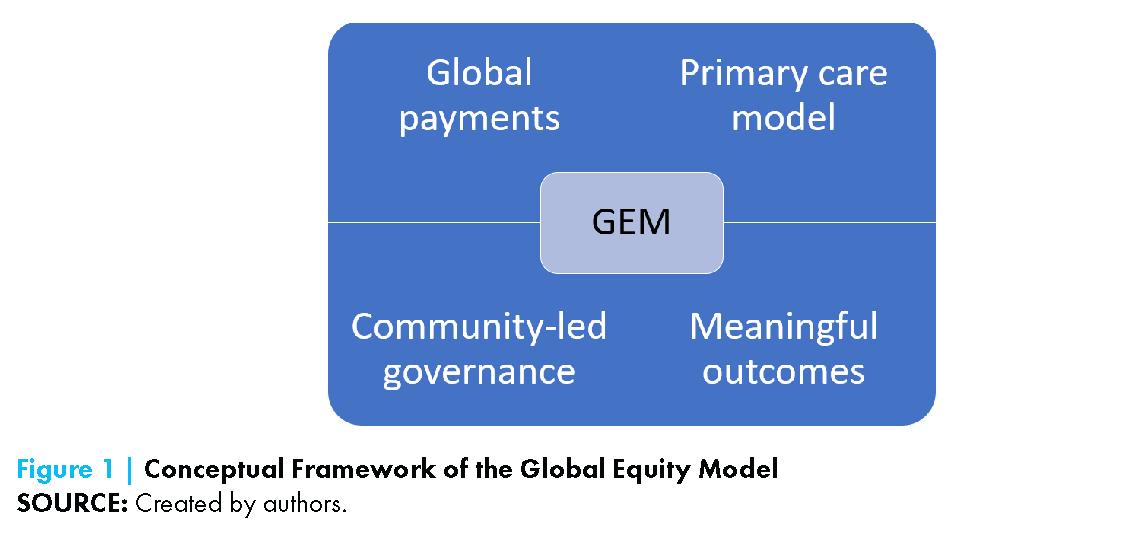

Component 1: Organization of Health System Payments in the GEM Program
All large health care systems within the health equity region should receive a global payment to cover care provided to the region’s residents. The payment model should, at a minimum, include publicly insured (including Medicare and Medicaid) and uninsured/self-pay individuals, who represent a majority of patients. Medicare Advantage participation will be especially crucial given its projected enrollment over the next decade, strong bipartisan and bicameral support of the program, and high participation rates in many areas where health disparities are prevalent (Agarwal et al., 2021). Private sector purchasers (i.e., self-insured employers), state employee health plans, health insurance exchange participants, and commercial payers should be added to the model as early as possible to ensure the necessary harmonization of performance metrics and population base required to drive clinical transformation is in place.
Initial Payment Amount
Health systems would receive a global payment for the care of residents who live in the region. The payment amount for each health system should be proportionate to service utilization, patient volume, and past revenue. Adjustments should be made to the initial payment amount to account for historical underpayment and under-resourced health systems. The latter can be identified by quantifying relative operating losses in the pre-model period relative to state or national averages, accounting for pre-model payment levels relative to cost. The initial health system payment amount should include supplementary payments and subsidies to sustain safety net health systems.
One-Time Foundational Payments to Health Systems
Beyond the global payment for health services, the model should provide one-time payments to support investments in infrastructure to support equity-based transformation in financially vulnerable institutions. These investments might include information technology and care management infrastructure. To finance these payments, CMS could use funds anticipated to be saved throughout the GEM program or identify the funds from outside the model for the explicit purpose of building capacity for equity. For example, Medicaid waivers and funding should be optimized, and grant funding or low-interest, forgivable loans may be provided through Health Resources and Services Administration.
These payments should be coordinated with additional resources for community organizations to address SDoH, including housing stability, food insecurity, and transportation. The federal government could coordinate the work of multiple departments to achieve this initial investment.
Payment Adjustments
Adjustments to health system payments should be made annually to account for changes in the size of the local population, wages, inflation, and unanticipated shifts in patient volume for services that are part of the global payments. As in the Maryland all-payer model, quality and outcomes-based payments should be made annually. Inflation adjustments should reflect the anticipated growth in the market basket of health care inputs. Quality and outcomes-based payments should be aligned with the model’s objectives of improving population health, reducing disparities, and reducing avoidable utilization and costs. Payment adjustments should facilitate the transition of resources to investments in community health services and the SDoH.
What Is in and What Is Out
The global payments for health systems should cover, at a minimum, all inpatient and outpatient hospital revenues for the population in the health equity region. Professional fees for some provider groups, such as hospital-employed physicians, can also be incorporated into the health system payment amount. Including only some physicians in a global payment may create significant challenges due to physician employment trends and shifts in service mix. Still, there is some precedent for physician reimbursement through hospital payments, as in the case of Critical Access Hospitals, with billing for specific physicians included in the hospital’s claims.
Implementation
There are two options for establishing and implementing global budgets for health systems. The first would be to use the Medicare rate system as the underlying accounting framework. Essentially, each participating payer would pay Medicare rates, adjusted by an agreed-upon multiplier. Medicare rates would then be adjusted in tandem up or down over the year so that the intended revenue reaches the hospital.
This approach has several advantages. First, it would provide for the correct revenue during the fiscal year, avoiding the need for a complicated reconciliation process at the year’s end. Second, it would clarify how Medicare Advantage plans and other smaller payers can participate; each would get a multiplier that would determine the rates to be paid. Third, it would support rational billing for the uninsured. The uninsured would be charged an allowed price with a multiplier that mirrors the Medicare rate, subject to charity care policies. In the setting of global revenues and multipliers, it would be anticipated that a significant fraction of billings for the uninsured would not be paid.
As preventable admissions decline, the corresponding rise in rates might be excessive. In this scenario, dividing payments into payments for investments in community health initiatives and rates related to clinical care costs might make sense.
The second option would be for Medicare, Medicaid, and private payers to provide fixed payments for the covered services and enrollees, adjusted for changes in membership and shifts of services among health systems. Such a fixed payment approach would have some potential appeal for administrative simplicity. Still, without a specific rate structure, it might be more challenging to require and secure the participation of Medicare Advantage and Medicaid managed care organizations on equal footing with other payers. Additionally, this second option would require periodic reconciliation and settlements. Regardless of the approach for implementing global budgets, hospital margins should be driven by growth in operating expenses against the fixed health system revenues and performance concerning efficiency, quality, and equity-based metrics.
Patients Outside of the Geographic Area
Many health systems have a stable number of patients seeking care outside their local communities. Incorporating payments for these patients in the GEM program is unnecessary. It would be possible for the GEM program to include revenue for these patients in the global payment. Close monitoring of trends is important in this case to avoid undermining the program. This share of the global payment budget should increase or decrease based on patient volumes from outside the health equity region except for volume reductions for avoidable use.
Total Cost of Care
The GEM program should closely monitor the per capita total cost of care for people in the health equity region, including the share of their care delivered outside the region. If the total cost of care exceeds a pre-specified benchmark, anticipating long-term savings, further investigation and modifications to the model should be considered. Health systems should receive a payment adjustment for a total cost of care performance, but it should be limited to a modest percentage of payments while health systems adapt to global payments, with the rate growing after the fifth year of the model. As the costs stabilize over the first several years, benchmarks for the total cost of care can be updated.
Vigilance will be necessary to reach the total cost of care goals. Shifts of services from hospitals to non-hospital settings must not generate duplicate expenditures. Caution should be taken to avoid excessive expense growth outside the health system payment, such as post-acute care. Unjustified variation in use relative to adjusted historical trends might be accounted for via adjustments to global payments if the growth was due to cost shifting.
Patient cost-sharing liability should be closely associated with a total cost of care performance. Meaningful reductions should also be translated to lower out-of-pocket cost obligations across all types of health care services, including inpatient facilities, ED visits, and other hospital outpatient departments and professional services.
Specialty Care
GEM should also entail accountability for the cost and outcomes associated with specialty care. For specialty providers employed by or affiliated with health systems, the GEM should track the cost of treatment episodes across all sites of care and span diagnosis to treatment to recovery. Modeled after the Bundled Payment for Care Improvement program, GEM-participating hospitals should be able to select from multiple condition-based clinical episodes and receive additional payments if total 90-day episode-based costs of care fall below peer benchmarks.
Savings Calculation
By reducing preventable illness, the GEM program should generate a favorable and consistent savings calculation against benchmarks for participating health care systems over time. This will engender a positive feedback loop with the community via investments in the community, non-primary care services, and programs to support equity-based care transformation. The model should calculate such savings up-front within the Medicare program by comparing Medicare-per-beneficiary total hospital cost growth rates between participating regions and matched geographical catchment areas or national spending trends. Through the community-led governance process described below, the GEM program should facilitate the reinvestment of a large portion of these savings back into communities, either in an amortized fashion or lump sum up front, to address health improvement and equity following the transformation plan.
Downside financial risk should not jeopardize the economic sustainability of safety-net institutions during the phase-in period of a geographic model. A phased-in approach to downside risk over the first several years should initially insulate health systems and appropriately incentivize them as they become more familiar with the GEM program and gain momentum with implementing their equity-transformation agenda.
Component 2: Primary Care
The GEM program should include a robust primary care component. High-quality and broadly accessible primary care supports population health through prevention and care management for individuals with chronic conditions and high social needs. Each health equity region should adopt a primary care model that (1) supports the continuity of care; (2) incentivizes disease prevention and wellness; (3) empowers primary care providers to provide care in alternate settings, such as through telemedicine, school-based clinics and home-based visits, as opposed to the traditional hospital setting; and (4) promotes a culture of continuous improvement in quality and patient experience.
The GEM should accommodate different options for primary care models. The primary care component might stand alone or be part of an ACO, with voluntary participation similar to existing programs. The model’s technical assistance and initial funding should include training, coaching, and investments in enabling infrastructures, such as information technology (IT) platforms, video technology, and dashboards. Existing CMS programs for primary care and IT, including accountable health communities, could guide these types of supports. At least a portion of additional investments should be provided through a risk-and area-level deprivation-adjusted monthly fee, creating revenue stability as practice transformation occurs. In some health equity regions, a statewide primary care model already exists and can be adapted readily for use in the region.
Care Management
The primary care component should include a robust care management program to help address chronic diseases, including behavioral and mental health conditions that are exacerbated in populations with health disparities. Embedded within the primary care or ACO team’s workflow, care managers should assist patients with self-care strategies, support timely access to care, identify and engage patients at high risk for decompensation, and help mitigate precipitating risk factors (Hayes and McCarthy, 2016; Hong et al., 2014). Screening and response to SDoH should be implemented longitudinally in case management. An example is the Protocol for Responding to and Assessing Patients’ Assets, Risks, and Experiences, the most common screening tool for SDoH deployed by U.S. health plans and health systems (Hayes and McCarthy, 2016). Robust implementation of this or similar protocols such as ED transitions of care or diversion programs can help practices to identify and help address unmet social and behavioral health needs (Neven et al., 2012).
Federally Qualified Health Centers
Federally Qualified Health Centers (FQHCs) are critical access points for many people to high-quality primary care and other services. Unfortunately, some existing primary care models have limited participation of FQHCs due to the complexity of their reimbursement. In the GEM program, FQHCs should be included and given access to a dedicated funding stream (derived from program savings or separately provided by the federal government) to enhance or expand their services as part of the overall community health equity plan.
Financial Incentives
The primary care model should include outcomes and cost of care incentives, recognizing that all of the model savings should not accrue to the health systems. First, outcomes incentives should align with population health and disparity reduction goals. These incentives should be paid regardless of the total cost of care. Improvement in health outcomes and health disparities can be expected to reduce avoidable utilization over time, and rewarding these outcomes consistently is a long-term investment in the model’s success.
Second, cost of care incentives should be tied to reductions in avoidable utilization and total cost of care performance. As the model matures, a portion of savings from reduced utilization should be designated to be shared with primary care practices that meet performance metrics. The total cost of care incentives, which are typically more challenging to manage with smaller practices due to the high variability of individual member costs, should be used in combination with utilization incentives. The development and application of cost of care incentives should also consider the local market structure of physician practices to facilitate collaboration by both independent and health system-aligned practices.
Larger financial incentives should be provided as greater improvements are seen. This is conceptually akin to the strategy used in Massachusetts under the Blue Cross Blue Shield Alternative Quality Contract, wherein a range of performance targets (“gates”) was created. Across the range of gates, each increment was associated with higher payment distribution (Jaffery and Safran, 2021). There should also be larger outcome incentives tied to improvements in health, community access and reductions in disparities, and incentives tied to the cost of care. Health outcome incentives should be aligned to the health system’s global payment approach to the extent feasible. Through these mechanisms, the GEM program will increase the availability, quality, and comprehensiveness of primary care in community settings.
Specialty Care Outside of Health Systems
As more patients obtain primary care, the demand for outpatient specialist care (e.g., radiology, ambulatory surgery) is likely to grow. This may exacerbate a shortage in outpatient specialty services in many areas already experiencing substantial health disparities. Similar to health professional shortage areas and rural health settings, specialists in health equity regions may experience financial challenges in providing services due to the high prevalence of Medicare and Medicaid patients with lower reimbursement rates, high uninsured, and lower proportions of higher-paying private patients. This can lead to a contracted supply of community-based services.
To help improve access and viability of community-based services, Medicaid and Medicare should offer incentives, such as increased reimbursement, for essential specialty services that are in short supply in the health equity region. These could be provided through the GEM or a parallel effort. Doing so would mitigate the need for uninsured and Medicaid enrollees to access outpatient services in the higher-cost hospital setting or outside the region entirely.
Component 3: Community Engagement and Empowerment
The GEM program should include a governance process that empowers the local community. This process should develop and oversee a community health transformation plan that emphasizes improving health equity and allows for the efficient and effective administration of the payment model.
Community-Led Governance
Each health equity region should have a community-led steering committee that oversees the development of a transformation plan. This plan aims to provide a path for improved health and well-being in the region.
The plan should be developed through broad public participation. It should identify primary focus areas such as maternal health, birth outcomes, school success, adolescent engagement, mental illness, lead exposure, school readiness, substance use disorders, and preventable chronic illness (i.e., heart disease, chronic obstructive pulmonary disease, and diabetes). The process should provide opportunities for all community stakeholders to have a voice and include culturally and linguistically appropriate avenues for participation. This community-led process should consist of the selection of region-specific metrics that will govern the model and be guideposts for efforts both inside and outside the health care system.
The plan should include clarity and transparency about how participating health systems intend to use novel financial incentives. These health equity region-specific plans should include planned changes to service lines to better align with community health. Emerging metrics for how hospitals can contribute to community health and equity—including through their roles as anchor institutions—can assist with this work (Plott et al., 2022). So too can experience with Coordinated Care Organizations in Oregon (McConnell, 2016). Pennsylvania requires concurrent transformation plans for each system as they enter into global budget arrangements, a process being updated to enhance broader stakeholder participation.
Beyond the health care system, the plan should include opportunities to align other health, economic, and social service programs with its goals. Participation in this process and on the steering committee should go beyond health care and include local nonprofit organizations, community leaders, businesses, and others. Key areas of focus should include housing availability and eviction prevention, food security, transportation access, and others.
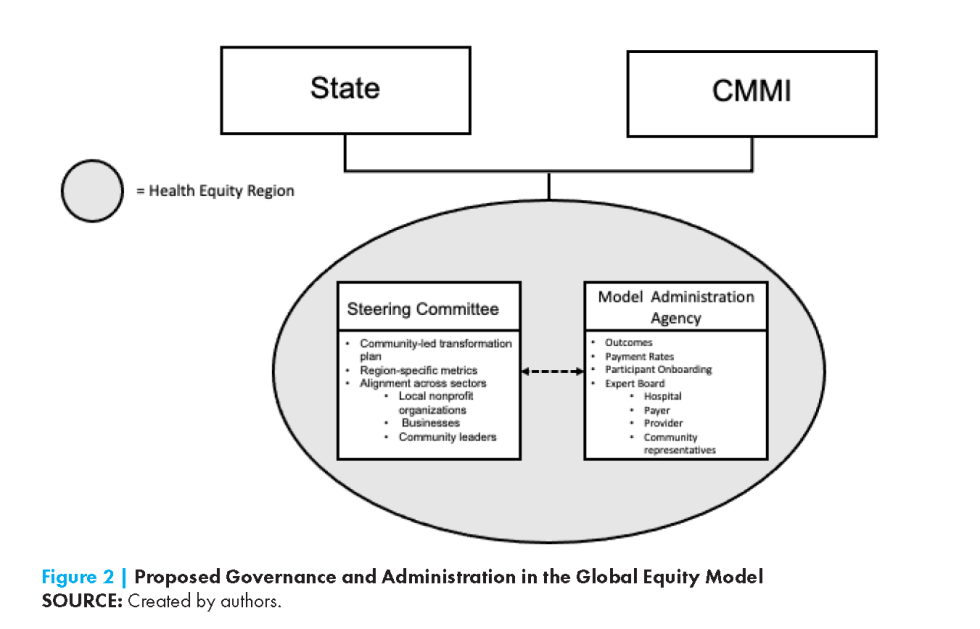
Administration of the Payment Model
Model administration should be the primary responsibility of an agency or organization jointly designated by CMMI and the state health department (see Figure 2). The administrative organization should be tasked with calculating the baseline payments, making periodic adjustments, onboarding participating payers and hospitals, establishing annual hospital-specific rates, overseeing data collection, assessing outcome metrics, and preparing key reports. This administrative entity should be governed by an expert board that includes hospital, payer, provider, and community representatives. Maryland, Vermont, and Pennsylvania all use a government instrumentality established through state legislation to administer their APMs, working together with CMMI. While the agencies/instrumentalities in each state have differing authorities, Medicaid participates in each of these states’ models. Strong state support and Medicaid participation are essential ingredients for success.
Role of States
States should make commitments to the health equity regions in their jurisdictions. First, the state’s Medicaid program should fully participate financially, requiring FFS and managed care payers to participate in global health system payment arrangements. Second, the state should gradually encourage and then require other payers to participate. As in Maryland, with its system of global hospital budgets, statutory language can ratify that the GEM program is the only health system payment mechanism for health equity regions, as this would ensure the participation of large self-funded employers and Medicare Advantage plans. Third, and critically, the state should organize its resources to accomplish the health goals in the covered areas through supporting transformation plans, health outreach, attention to SDoH, and other steps.
One such model is the health enterprise zone (HEZ) program in Maryland, which organized state resources to support locally developed initiatives that led to cost savings and reductions in inpatient stays (Khullar et al., 2020). Core components included the targeted recruitment of primary care physicians to economically deprived or health care-underserved regions, use of community health workers, and enhanced care coordination (Khullar et al., 2020). Of note, each HEZ is tailored to the unique social needs and care barriers salient to a particular reference population. Maryland has recently re-established the Health Equity Resource Community model based on the HEZ approach.
Another model is Rhode Island’s Health Equity Zone initiative, a health equity-centered approach to prevention work that leverages place-based, community-led solutions to address SdoH. Through a braided funding model, Rhode Island has invested more than $30 million in public health funding toward 15 Health Equity Zone collaboratives to develop sustainable infrastructure and support community-identified needs to positively impact the socioeconomic and environmental conditions driving disparities and improve health outcomes (Patriarca and Ansura, 2016).
Other Federal Agencies
Other federal agencies should align their efforts in the health equity regions by supporting access to grant programs, loaned staff, tax credits, and other resources. Such investments should not be part of the savings calculations for the model; these are simply other available resources that can leverage more systemic change by aligning with the goals and efforts of the GEM program. An example of how additional federal resources can be leveraged for place-based initiatives is the Health Enterprise Zones Act, sponsored by Congressman Anthony G. Brown (Agarwal et al., 2021).
Component 4: Data, Outcome, and Performance Metrics
A robust data infrastructure is critical for model success, meaningful care transformation, and long-term sustainability. The Maryland Global Budget model offers several key implementation lessons. First, a statewide health information exchange (HIE) is a foundational first step for generating actionable insights. Second, special arrangements with CMS and commercial payers should be put in place to expedite data sharing and quality reports with the participating health systems. Ideally, this information should encompass health plans, personal health information, utilization history, care plans, and medical history. Up-front funding should also be embedded in program design and savings calculation to allow health systems to fund necessary personnel and infrastructure to house, curate, merge, and analyze the data (Kilaru et al., 2022).
The GEM program should leverage clear metrics to advance health equity and meet more traditional performance goals. Population health equity measurements should be sensitive enough to identify actual population-level gains while being contextually relevant to the needs of the population being served (Patel et al., 2021). Because the GEM focuses on the health of the entire population in the health equity region, the metrics should be all-payer. The metrics should also be vetted through the community governance process, be reported publicly, and become a focal point in the region’s transformation plan. Ideally, these metrics should cover the following areas.
Community Health
Core outcome metrics should be identified through the community planning process. As noted above, examples could include maternal health, birth outcomes, school success, adolescent engagement, mental illness, substance use disorders, and preventable chronic illnesses like heart disease, chronic obstructive pulmonary disease, and diabetes. CMS should consider requiring the inclusion of specific fundamental metrics such as life expectancy and infant mortality (Patel et al., 2021).
Preventive Services
Metrics to appropriately track the use of preventive services could include access to recommended screenings, primary care utilization, and vaccination uptake.
Utilization of Facility-Based Care
Metrics could include reductions in all-cause and unplanned hospital admissions, reductions in ER visits for ambulatory-sensitive conditions, decreases in institutional post-acute care, and concomitant increases in in-home health services or hospital-at-home models. The authors of this paper envision that participation in the GEM program could replace the CMS hospital quality reporting program for attributed health systems.
Health Disparity Goals
Goals should be set to close health disparities. Accordingly, metrics should be stratified and reported by race/ethnicity, gender, language, disability, and other relevant demographic dimensions and key geographic variables such as a neighborhood. Performance measurement should bring together various measures (process- and outcomes-based) to track progress in closing critical gaps. For example, if improving maternal health for Black women is a local focus, assembled metrics might reflect access to care (percent of Black pregnant women seen in the first trimester), process (screening rates for Black and Hispanic women at risk for pregnancy-related complications, lead exposure, kindergarten readiness), and outcomes (infant mortality, HbA1c levels among pregnant minority women with diabetes) (Hong et al., 2014).
Health Equity Goals
These metrics should encompass major social goals related to health, such as reducing homelessness, unemployment, food insecurity, and school absenteeism; improving school readiness; and enhancing community safety.
Care Quality
These metrics should include traditional quality metrics as appropriate and new measures recommended by CMMI and approved by the administrative agency. Ultimately, the metrics should replace the CMS hospital quality program requirements for participating hospitals.
Alignment of Metrics
Health systems and primary care providers should be subject to the same or similar outcome measures to judge their success in improving population health and reducing disparities. This alignment will support collaborative efforts across the community.
Implementation Timeline
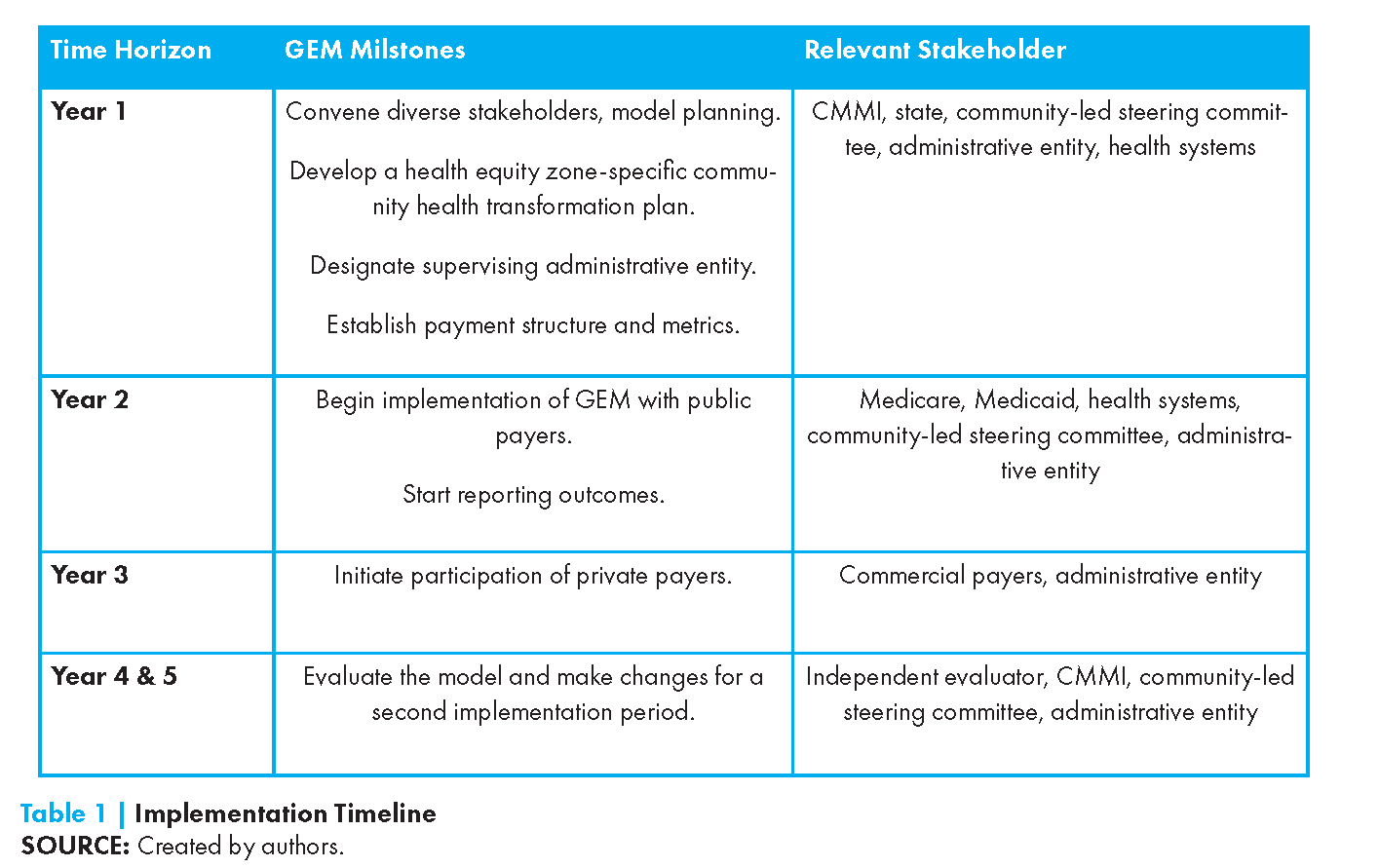
For many regions in the U.S., a three- to five-year transition period leading up to GEM implementation will be necessary to create the environmental conditions required for success (e.g., statewide HIE, the establishment of the administrative entity, technical assistance for IT infrastructure, and generating hospital buy-in). The GEM should be implemented over a five- to seven-year period, with year one for model planning; years two to three to establish the administrative agency, health care payment structures, and metrics; and years four to five to begin fully implementing the model (see Table 1). An updated plan is necessary to maintain investment and support to ensure model continuation after this “incubation” period.
Limitations
We see three primary limitations of this model. First, the model requires a strong sense of community across health systems, community organizations, public health agencies, and political leadership. Without a common cause, the GEM is not likely to be successful. Second, the model requires effective and nimble use of data. Success will require upgrading systems and establishing pathways for effective data sharing. Third, the model’s progress depends on aligned efforts inside and outside government at the local, state, and national levels. Payment reform alone will not be sufficient to accomplish the ambitious goals that stretch beyond the health care system’s reach. Because of these limitations, we do not believe that this model can be imposed on regions without their full participation. With sufficient incentives, however, the model can spark regional cooperation and commitment to make it successful.
Next Steps
CMS should gauge broad stakeholder interest in potential GEM implementation and receive input on model design through public meetings and calls for information. Mobilizing payers, providers, patient groups, researchers, policy makers, and others in a shared mission will increase the focus on and accountability for health equity.
Join the conversation!
Tweet this! Authors of a new #NAMPerspectives discussion paper propose a Global Equity Model payment framework to improve community health and health equity by reducing preventable illness and use the savings to invest in social drivers of health. Read more: https://doi.org/10.31478/202211b
Tweet this! In a new #NAMPerspectives, authors assess existing reimbursement frameworks, propose a Global Equity Model payment framework, and lay out an implementation timeline to create the environmental conditions required for success. Read more: https://doi.org/10.31478/202211b
Tweet this! “Recent payment innovations have shown promise and provide an important foundation for even more ambitious payment models that improve community health and equity as a fundamental objective.” Read more: https://doi.org/10.31478/202211b
Download the graphics below and share them on social media!
References
- Agarwal, R., J. Connolly, S. Gupta, and A. S. Navathe. 2021. Comparing medicare advantage and traditional Medicare: A systematic review. Health Affairs 40(6):937-944. https://doi.org/10.1377/hlthaff.2020.02149.
- Anderson, R. E., J. Z. Ayanian, A. M. Zaslavsky, and J. M. McWilliams. 2014. Quality of care and racial disparities in Medicare among potential ACOs. Journal of General Internal Medicine 29(9):1296-1304. https://doi.org/10.1007/s11606-014-2900-3.
- Baker, M. C., P. M. Alberti, T. Y. Tsao, K. Fluegge, R. E. Howland, and M. Haberman. 2021. Social determinants matter for hospital readmission policy: Insights from New York city. Health Affairs 40(4):645-654. https://doi.org/10.1377/hlthaff.2020.01742.
- Braveman, P., E. Arkin, T. Orleans, D. Proctor, and A. Plough. 2017. What Is Health Equity? And What Difference Does a Definition Make? Princeton, NJ: Robert Wood Johnson Foundation.
- Center for Medicare & Medicaid Innovation (CMMI). Evaluation of the Vermont All-Payer Accountable Care Organization—First Evaluation Report. Available at: https://innovation.cms.gov/data-and-reports/2021/vtapm-1st-eval-full-report.
- Center for Medicare and Medicaid Innovation (CMMI). 2021b. The Pennsylvania Rural Health Model – First Annual Report. Available at: https://innovation.cms.gov/data-and-reports/2021/parhm-ar1-full-report.
- Center for Medicare and Medicaid Services. 2019. Evaluation of the Maryland All-Payer Model. Volume 1: Final Report. Available at: https://downloads.cms.gov/files/md-allpayer-finalevalrpt.pdf.
- Center for Medicare and Services. 2020. Accountable Health Communities (AHC) Model Evaluation—First Evaluation Report. Available at: https://innovation.cms.gov/data-and-reports/2020/ahc-first-eval-rpt.
- Centers for Medicare & Medicaid Services (CMS). 2021. Innovation Center Strategy Refresh. Available at: https://innovation.cms.gov/strategic-direction-whitepaper.
- Fraze, T. K., E. S. Fisher, M. R. Tomaino, K. A. Peck, and E. Meara. 2018. Comparison of Populations Served in Hospital Service Areas With and Without Comprehensive Primary Care Plus Medical Homes. JAMA Network Open 1(5):e182169. https://doi.org/10.1001/jamanetworkopen.2018.2169.
- Hayes, S., and D. McCarthy. 2016. Care Management Plus: Strengthening primary care for patients with multiple chronic conditions. Commonwealth Fund. Available at: https://www.commonwealthfund.org/publications/case-study/2016/dec/care-management-plus-strengthening-primary-care-patients-multiple
- Hong, C. S., A. L. Siegel, and T. G. Ferris. 2014. Caring for high-need, high-cost patients: what makes for a successful care management program? Issue Brief (Commonwealth Fund). Available at: https://www.commonwealthfund.org/publications/issue-briefs/2014/aug/caring-high-need-high-cost-patients-what-makes-successful-care.
- Jaffery, J., and D. Safran. 2021. Addressing social risk factors in value-based payment: Adjusting payment not performance to optimize outcomes and fairness. Health Affairs Blog. Available at: https://www.healthaffairs.org/do/10.1377/forefront.20210414.379479/full/.
- Joynt, K. E., N. De Lew, S. H. Sheingold, P. H. Conway, K. Goodrich, and A. M. Epstein. 2017. Should Medicare Value-Based Purchasing Take Social Risk into Account? New England Journal of Medicine 376(6):510-513. https://doi.org/10.1056/NEJMp1616278.
- Khullar, D., Y. Zhang, and R. Kaushal. Potentially Preventable Spending Among High-Cost Medicare Patients: Implications for Healthcare Delivery. Journal of General Internal Medicine 35(10):2845-2852. https://doi.org/10.1007/s11606-020-05691-8.
- Kilaru, A. S., C. R. Crider, J. Chiang, E. Fassas, and K. J. Sapra. 2022. Health Care Leaders’ Perspectives on the Maryland All-Payer Model. JAMA Health Forum 3(2):e214920. https://doi.org/10.1001/jamahealthforum.2021.4920.
- Kim, H., T. H. A. Meath, F. W. Tran, A. R. Quiñones, K. J. McConnell, and S. A. Ibrahim. 2020. Association of Medicare Mandatory Bundled Payment System for Hip and Knee Joint Replacement with Racial/Ethnic Difference in Joint Replacement Care. JAMA Network Open 3(9):e2014475. https://doi.org/10.1001/jamanetworkopen.2020.14475.
- Kim, H., T. H. A. Meath, F. W. Tran, A. R. Quiñones, K. J. McConnell, and S. A. Ibrahim. 2021. Association of Medicare Mandatory Bundled Payment Program with the Receipt of Elective Hip and Knee Replacement in White, Black, and Hispanic Beneficiaries. JAMA Network Open 4(3):e211772. https://doi.org/10.1001/jamanetworkopen.2021.1772.
- LaVeist, T. A., D. Gaskin, and P. Richard. 2011. Estimating the economic burden of racial health inequalities in the United States. International Journal of Health Services 41(2):231-238. https://doi.org/10.2190/HS.41.2.c.
- Lewis, V. A., C. H. Colla, K. L. Carluzzo, S. E. Kler, and E. S. Fisher. 2013. Accountable care organizations in the United States: Market and demographic factors associated with formation. Health Services Research 48(6 Pt 1):1840-1858. https://doi.org/10.1111/1475-6773.12102.
- Lewis, V.A., T. Fraze, E. S. Fisher, S. M. Shortell, and C. H. Colla. 2017. ACOs serving high proportions of racial and ethnic minorities lag in quality performance. Health Affairs 36(1):57-66. https://doi.org/10.1377/hlthaff.2016.0626.
- Magesh, S., D. John, W. T. Li, Y. Li, A Mattingly-app, S. Jain, E. Y. Change, and W. M. Ongkeko. 2021. Disparities in COVID-19 Outcomes by Race, Ethnicity, and Socioeconomic Status: A Systematic-Review and Meta-analysis. JAMA Network Open 4(11):e2134147. https://doi.org/10.1001/jamanetworkopen.2021.34147.
- Markovitz, A. A., J. M. Hollingsworth, J. Z. Ayanian, E. C. Norton, N. M. Moloci, P. L. Yan, and A. M. Ryan. 2019. Risk adjustment in medicare ACO program deters coding increases but may lead ACOs to drop high-risk beneficiaries. Health Affairs 38(2):253-261. https://doi.org/10.1377/hlthaff.2018.05407.
- Masters, S. H., R. I. Rutledge, M. Morrison, H. A. Beil, and S. G. Haber. 2022. Effects of Global Budget Payments on Vulnerable Medicare Subpopulations in Maryland. Medical Care Research Review 79(4):535-548. https://doi.org/10.1177/10775587211052748.
- 2021. Evaluation of the Maryland Total Cost of Care Model: Implementation Report. Available at: https://innovation.cms.gov/data-and-reports/2021/md-tcoc-imp-eval-report.
- McConnell, K. J. 2016. Oregon’s medicaid coordinated care organizations. JAMA 315(9):869-870. https://doi.org/10.1001/jama.2016.0206.
- McKenzie, J. F., R. R. Pinger, and J. E. Kotecki. 2005. An Introduction to Community Health. Sudbury, MA: Jones and Bartlett Learning.
- Murray, G. F., H. P. Rodriguez, and V. A. Lewis. 2020. Upstream with a small paddle: How ACOs are working against the current to meet patients’ social needs. Health Affairs 39(2):199-206. https://doi.org/10.1377/hlthaff.2019.01266.
- Murray, R. 2009. Setting hospital rates to control costs and boost quality: The Maryland experience. Health Affairs 28(5):1395-1405. https://doi.org/10.1377/hlthaff.28.5.1395.
- Neven, D., J. Sabel, and D. Howell. 2012. Robust implementation of this or similar protocols can help practices to identify and help address unmet social needs. Journal of Medical Toxicology 8(4):353-359.
- Nussbaum, S., M. McClellan, and G. Metlay. 2018. Principles for a Framework for Alternative Payment Models. JAMA 319(7):653-654. https://doi.org/10.1001/jama.2017.20226.
- Offodile, A. C., W. Mehtsun, C. J. Stimson, and T. Aloia. 2019. An Overview of Bundled Payments for Surgical Oncologists: Origins, Progress to Date, Terminology, and Future Directions. Annals of Surgical Oncology 26(1):3-7. https://doi.org/10.1245/s10434-018-7037-x.
- Papanicolas, I, L. R. Woskie, and A. K. Jha. 2018. Health Care Spending in the United States and Other High-Income Countries. JAMA 319(10):1024-1039. https://doi.org/10.1001/jama.2018.1150.
- Patel, S., A. Smithey, K. Tuck, and T. McGinnis. 2021. Leveraging Value-Based Payment Approaches to Promote Health Equity: Key Strategies for Health Care Payers. Center for Healthcare Strategies. Available at: https://www.chcs.org/resource/leveraging-value-based-payment-approaches-to-promote-health-equity-key-strategies-for-health-care-payers/.
- Patriarca, M., and C. J. Ausura. 2016. Introducing Rhode Island’s Health Equity Zones. Rhode Island Medical Journal 99(11):47-48.
- Plott, C. F., R. L. J. Thornton, E. Punwani, I. Dankwa-Mullan, H. Karimalara, K. J. T. Craig, K Rhee, and J. M. Sharfstein. 2022. The development and implementation of a new hospital performance measure to assess hospital contributions to community health and equity. Health Services Research. https://doi.org/10.1111/1475-6773.14018.
- Samuel, L. J., D. J. Gaskin, A. J. Trujillo, S. L. Szanton, A. Samuel, and E. Slade. 2021. Race, ethnicity, poverty and the social determinants of the coronavirus divide: U.S. county-level disparities and risk factors. BMC Public Health 21(1):1250. https://doi.org/10.1186/s12889-021-11205-w.
- Schpero, W. L., N. E. Morden, T. D. Sequist, M. B. Rosenthal, D. J. Gottlieb, and C. H. Colla. 2017. Datawatch: For selected services, blacks and hispanics more likely to receive low-value care than whites. Health Affairs 36(6):1065-1069. https://doi.org/10.1377/hlthaff.2016.1416.
- Seshamani, M., and D. Jacobs. 2022. Leveraging Medicare to Advance Health Equity. JAMA 327(18):1757-1758. https://doi.org/10.1001/jama.2022.6613.
- Stephenson, J. 2022. Medical Debt Burdens Millions of U.S. Adults. JAMA Health Forum 3(3):e220910. https://doi.org/10.1001/jamahealthforum.2022.0910.
- Sze, S., D. Pan, C. R. Nevill, L. J. Gray, C. A. Martin, J. Nazareth, J. S. Minhas, P. Divall, K. Khunti, K. R. Abrams, L. B. Nellums, and M. Pareek. Ethnicity and clinical outcomes in COVID-19: A systematic review and meta-analysis. eClinicalMedicine. https://doi.org/10.1016/j.eclinm.2020.100630.
- The Commonwealth Fund. 2019. U.S. Health Care from a Global Perspective, 2019: Higher Spending, Worse Outcomes? Available at: https://www.commonwealthfund.org/publications/issue-briefs/2020/jan/us-health-care-global-perspective-2019.
- Vasquez Reyes, M. 2020. The Disproportional Impact of COVID-19 on African Americans. Health and Human Rights 22(2):299-307.
- Yasaitis, L. C, W. Pajerowski, D. Polsky, and R. M. Werner. 2016. Physicians’ participation in ACOs is lower in places with vulnerable populations than in more affluent communities. Health Affairs 35(8):1382-1390. https://doi.org/10.1377/hlthaff.2015.1635.
- Zuvekas, S. H., and J. W. Cohen. 2016. Datawatch: Fee-for-service, while much maligned, remains the dominant payment method for physician visits. Health Affairs 35(3):411-414. https://doi.org/10.1377/hlthaff.2015.12.


